Medical billing software shapes how fast your practice gets paid, how many claims get denied, and how much time your team spends chasing revenue instead of delivering care. However, in a crowded market where pricing and features are often unclear, it can be difficult to know which product will best suit your needs.
Most "top 10" online medical billing software lists read like vendor brochures rather than practical buying guides. We take the opposite approach in this article. Our detailed guide objectively evaluates leading products on key performance areas like claims workflow, denial management, reporting, integrations, and pricing transparency.
Whether you run a two-provider clinic or a multi-specialty hospital group, the goal is to help you match your billing needs to the platform that fits your operation. Keep reading for a comprehensive breakdown of the 10 best medical billing software products in 2026, followed by a step-by-step framework for making your final decision.
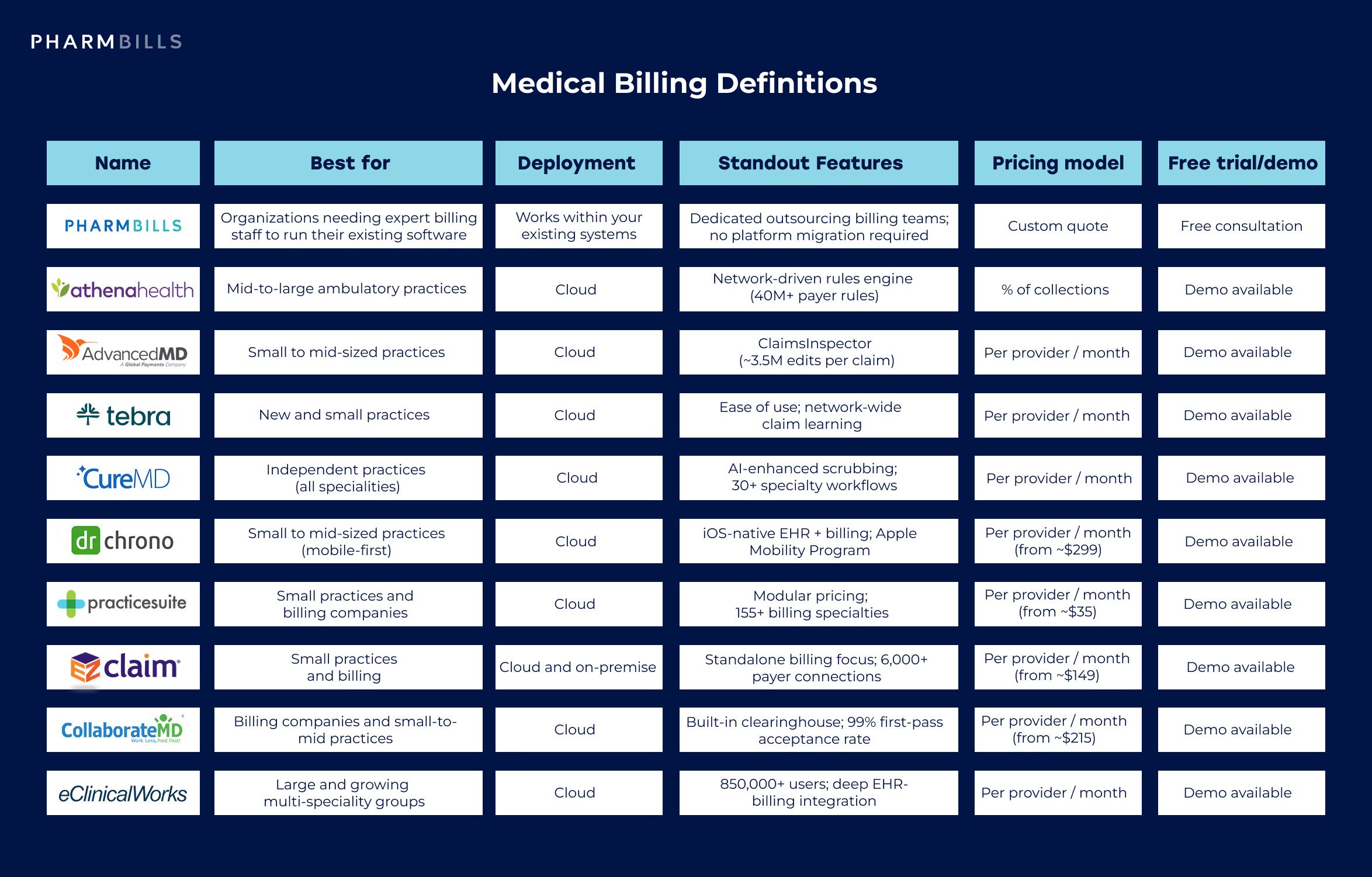
Best Medical Billing Software: Quick Comparison Table
The medical billing software comparison table below provides a high-level snapshot to help narrow your shortlist. After explaining how we evaluated vendors for this article, you’ll find detailed reviews of each of the products in the table.
How We Evaluated the Best Medical Billing Software
Medical billing software reviews only have value if the evaluation criteria reflect what matters in real-world billing operations. Rather than reviewing platforms in generic terms, we applied a 'best for' segmentation approach, matching each tool to the practice type, size, and workflow it serves best.
Here is how we assessed key performance domains of each platform before writing this article.
Claims Management and Scrubbing
We prioritized platforms with automated claim edits, real-time eligibility checks, payer-specific rule engines, and clear resubmission workflows. A clean claim rate above 95% on first pass was the baseline expectation.
Denial Management and Payment Posting
Effective denial tracking requires:
- Reason-code visibility
- Follow-up work queues
- Appeal workflow tools
- Support for electronic remittance advice (ERA) and explanation of benefits (EOB) processing
We evaluated how each platform handles the full denial lifecycle, from identification to resolution.
Reporting and Financial Visibility
Dashboards, A/R aging reports, payer performance breakdowns, and reimbursement trend analysis were all assessed. The best platforms allowed custom report building without requiring a dedicated analyst.
Integrations and Interoperability
The potential for reducing duplicate data entry is one of the main benefits of medical billing software. To assess this, we examined EHR compatibility, practice management (PM) system connections, clearinghouse relationships, patient payment tools, and lab or pharmacy integrations.
Pricing Transparency and ROI
Many vendors emphasize demos and custom quotes rather than publishing clear pricing. We gave credit to platforms that allow buyers to review medical billing software pricing to understand their likely costs before committing to a sales call.
More Information
For a detailed framework on evaluating billing partners—including KPIs, contract red flags, demo checklists, and more—see our full guide on How to Choose the Best Medical Billing Company.
Top Medical Billing Software Reviews for 2026

In the comparison of medical billing software below, all 10 platforms are reviewed in a consistent format:
- Overview (what it does)
- Best for (who it serves best)
- Key strengths
- Limitations
- Pricing
- Integration highlights
These detailed medical billing software reviews are based on vendor documentation, third-party review platforms, and operational analysis. Where pricing is not publicly available, we note this clearly.
1. Pharmbills — Best for When You Need Expert Staff on Your Billing Team
Overview: Pharmbills is an outsourced billing and revenue cycle staffing provider that places dedicated, trained professionals directly into your existing technology stack. Pharmbills appears first in this guide because software is only half the billing equation—the other half is having skilled people to operate it effectively.
Best for: Organizations that need expert billing staff to operate their existing software.
Key strengths:
- Zero workflow disruption. Pharmbills teams work inside whatever system your organization uses (Epic, eClinicalWorks, athenahealth, AdvancedMD, or any other platform). No migration required.
- Proven financial impact. One client operating 97 nursing home facilities saved over $5,000,000 in nine months after Pharmbills staff identified widespread outpatient claims errors and built a dedicated claims audit function.
- Rapid scaling. Pharmbills can onboard up to 25 professionals per month, supporting organizations through rapid growth without the delays of domestic hiring.
- Dedicated retention programs. Top talent is retained through structured mentoring, proactive issue resolution, and appreciation programs, reducing the turnover that often disrupts billing continuity.
Limitations: Pharmbills does not provide proprietary billing software. Organizations need their own technology stack. This is by design, as it gives you full control over your platform choice.
Pricing: Custom quote based on team size, scope, and system complexity. Clients typically reduce operational labor costs by 40–50% compared to domestic staffing.
Verdict: The strongest fit for organizations that want to maximize return on their billing software by pairing it with skilled human operators at a fraction of local staffing costs.
2. athenahealth — Best for Network-Driven Revenue Cycle Performance
Overview: athenahealth delivers an integrated EHR, practice management, and billing platform through athenaOne. Its core differentiator is network intelligence, which claims to have data from over 160,000 providers that feeds a continuously updated rules engine.
Best for: Mid-sized ambulatory practices (1–75 providers).
Key strengths: The rules engine contains over 40 million payer-specific rules and supports a first-pass claim acceptance rate above 95%. athenahealth earned #1 Best in KLAS 2026 for Practice Management for multiple consecutive years. Implementation averages 11 weeks.
Limitations: The RCM service is tightly coupled with athenahealth's EHR, meaning it is not a standalone billing solution for organizations using a different system. Percentage-of-collections pricing can become expensive for high-revenue practices.
Pricing: Percentage of monthly collections (reported range: 4–8%, though rates can reach higher depending on complexity). No upfront license fees.
Key integrations: 300+ marketplace integrations; direct connections to labs, pharmacies, and clearinghouses. FHIR-based interoperability.
Verdict: A strong choice if you want billing and clinical workflows unified under one cloud-native system, provided you're comfortable with percentage-based pricing that scales with revenue.
3. AdvancedMD — Best for Claim Accuracy
Overview: AdvancedMD offers cloud-based practice management, EHR, and billing services. They are known for a particular strength in pre-submission claim accuracy.
Best for: Small to mid-sized practices prioritizing claim accuracy.
Key strengths: The ClaimInspector module runs approximately 3.5 million edits per claim, and the company reports a first-pass claims rate of nearly 100%. AdvancedMD earned best-in-class recognition from SelectHub for medical billing and patient engagement.
Limitations: Does not include medical coding services (an in-house coder or third-party coding partner is required). May not support all specialties well, particularly physical therapy and behavioral health.
Pricing: Per provider per month. Third-party estimates suggest pricing in the range of $429–$729+ per provider, per month, depending on modules selected. Custom quotes required.
Key integrations: Clearinghouse connections, lab interfaces, and patient communication tools. EHR is included, but optional if using billing only.
Verdict: Ideal for practices that want aggressive automated scrubbing in a cloud-based package, but requires coding to be handled separately through an in-house coder or third-party partner.
4. Tebra (Formerly Kareo) — Best for Quick Setup and Ease of Use
Overview: Tebra combines practice management, EHR, claims tracking, and optional managed billing through third-party affiliates. It serves over 42,000 practices nationwide.
Best for: New and small practices prioritizing ease of use.
Key strengths: Recognized for exceptional ease of use and claims tracking transparency. The rules engine scrubs claims using network-wide learning, and the platform achieved high claim accuracy scores in third-party testing.
Limitations: Tebra does not directly handle billing services. Instead, it connects practices with third-party billing affiliates, which introduces variability in service quality. This means it may be better suited for standard workflows than complex specialty billing.
Pricing: Per provider, per month. Starting prices are available on request. Managed billing services are priced separately.
Key integrations: Integrates with multiple EHR systems, labs, and clearinghouses. Patient engagement tools are built in.
Verdict: A solid entry point for practices that need functional billing without a steep learning curve. Managed billing quality may vary since it's delivered through third-party affiliates, not Tebra directly.
5. CureMD — Best for AI-Enhanced Scrubbing Across 30+ Specialties
Overview: CureMD provides a cloud-based EHR, practice management, and RCM platform, with AI-enhanced claim scrubbing and support for over 30 specialty-specific workflows.
Best for: Independent practices wanting an affordable all-in-one platform.
Key strengths: CureMD reports a 99.9% claim acceptance rate that can help practices get paid up to 35% faster. AI-driven claim scrubbing and detailed KPI dashboards are included. MIPS compliance support is built in.
Limitations: Best suited for small to mid-sized independent practices. Larger health systems or organizations with complex multi-entity billing may find the platform limiting.
Pricing: Per provider per month. Custom quotes based on practice size and modules. Pricing is generally positioned as affordable relative to competitors.
Key integrations: Supports EHR, lab ordering, e-prescribing, and clearinghouse connections. API available for custom integrations.
Verdict: A solid option for independent practices that want billing, EHR, and compliance tools in a single platform, without enterprise-level complexity or cost.
6. DrChrono — Best for Billing and Charting from Mobile Devices
Overview: DrChrono is a cloud-based EHR, practice management, and billing platform built around mobile workflows. It was the first EHR to become an Apple Mobility Partner and offers full charting, scheduling, and billing from iPad, iPhone, or web.
Best for: Small to mid-sized practices that prioritize mobile workflows.
Key strengths: Billing profiles let providers pre-populate charge codes by visit type, reducing data entry significantly. Built-in claim scrubbing, real-time eligibility checks, and customizable reporting (including denial analysis, aging A/R, and collections breakdowns) are included. Full RCM outsourcing is available, and DrChrono includes clearinghouse fees in its RCM percentage—unlike many competitors that bill them separately.
Limitations: Practices using DrChrono's RCM services are required to use its EHR and practice management software (there is no standalone billing option). Some users report inconsistent customer support, and the platform's feature depth can feel excessive for very small or solo practices with simple billing needs.
Pricing: Per provider per month, starting from approximately $299. RCM services are priced as a percentage of collections (reported range: 3–9%), with the exact rate depending on specialty, volume, and practice size.
Key integrations: Connects with Updox, Square, Solv, and Birdeye. Lab integrations, e-prescribing with EPCS, and FHIR-based interoperability are built in. API access is available for custom integrations.
Verdict: The top pick for practices that prioritize mobile access and want billing, clinical, and patient engagement tools designed for on-the-go workflows. The requirement to use DrChrono's EHR for RCM services means it's an all-or-nothing commitment.
7. PracticeSuite — Best for Modular Billing Starting at $35/Month
Overview: PracticeSuite is a cloud-based practice management and billing platform supporting over 155 billing specialties and 60+ clinical specialties. It also serves third-party billing companies with multi-practice dashboard capabilities.
Best for: Budget-conscious practices and third-party billing companies.
Key strengths: Modular pricing lets practices pay for billing only or scale up to the full platform. The system includes real-time dashboards, claims management, collection management, and a patient portal. PracticeSuite reports over 57,000 medical professionals on the platform.
Limitations: Some users report a dated interface and a learning curve when navigating multiple modules. AI capabilities are still evolving.
Pricing: Per provider subscription starting from approximately $35 per month, making it one of the most affordable options in the market. Training and a dedicated success coach are included.
Key integrations: Connects with labs, pharmacies, HIE networks, and the patient portal. EHR is available but optional.
Verdict: The go-to option for practices and billing companies that want full-featured billing at the lowest monthly entry point in this guide — especially relevant when a medical billing software for third party billing companies prices comparison is driving the decision.
8. EZClaim — Best for Standalone Billing With Flexible Deployment
Overview: EZClaim is a billing and scheduling platform designed specifically for small to medium-sized practices and outsourced billing firms. It offers both cloud-based and on-premise deployment options.
Best for: Small practices and billing companies wanting standalone billing.
Key strengths: Processes over 4 million claims per month. Supports 6,000+ payer connections, automated claim scrubbing, ERA auto-posting, and customizable templates. US-based customer support receives consistently strong reviews.
Limitations: Does not include a built-in EHR—must integrate with third-party systems such as Practice Fusion, WebPT, or Elation Health. No API available, which may limit custom integrations. No weekend or after-hours support.
Pricing: Subscription starting from approximately $149 per month. Free trial available. No long-term contracts required.
Key integrations: Integrates with Practice Fusion, Amazing Charts, WebPT, Elation Health, BestNotes, and multiple clearinghouses.
Verdict: A strong pick for medical billing software for small practices and billing companies that want a focused, affordable billing tool. The lack of a built-in EHR and no API access may limit practices with more complex integration needs.
9. CollaborateMD — Best for Practices Wanting a Built-In Clearinghouse
Overview: CollaborateMD is a cloud-based practice management and billing platform with a built-in clearinghouse, real-time claim submission, and tools designed for both healthcare practices and billing service companies.
Best for: Billing companies and small-to-mid practices wanting a built-in clearinghouse.
Key strengths: Reports a 99% first-pass claim acceptance rate. Built-in clearinghouse can accelerate claims resolution and may provide deeper claim-level visibility. Offers 125+ reports with customizable dashboards, patient payment plans, prompt-pay discounts, and unlimited users.
Limitations: Not an EHR. CollaborateMD requires integration with external clinical systems. Scheduling features are considered basic.
Pricing: Per provider per month, starting from approximately $215 for practices and $235 for billing companies. Four plan tiers available (Starter, Basic, Growth, Unlimited).
Key integrations: Bidirectional interfaces with Elation, Practice Fusion, WebPT, Kipu, Amazing Charts, Sevocity, Praxis EMR, and others.
Verdict: A top-tier choice for medical billing software for clinics and billing companies that value integrated clearinghouse access and strong reporting.
10. eClinicalWorks — Best for Enterprise EHR-Billing Integration at Scale
Overview: eClinicalWorks (eCW) is one of the most widely deployed EHR and practice management platforms in the United States, serving over 850,000 medical professionals and 180,000 physicians.
Best for: Large and growing multi-specialty groups, health centers, and hospital-affiliated practices that need deep EHR-billing integration and scalability.
Key strengths: Claims and billing data flow directly from clinical documentation, helping to reduce coding errors. Built-in RCM services are available for practices that want to outsource billing without leaving the eCW ecosystem. Telehealth billing integration is included.
Limitations: The interface can be cluttered and difficult for first-time users. Some user reviews cite slow customer support response times and hidden add-on costs that increase the total price significantly.
Pricing: Per provider per month. Published pricing starts around $449 for the full suite. Additional fees may apply for implementation, training, and add-on services.
Key integrations: Connects with labs, pharmacies, imaging services, clearinghouses, and third-party tools. Supports 50+ specialty-specific templates.
Verdict: A comprehensive choice for organizations that need billing tightly woven into an enterprise-scale EHR. Among the platforms we reviewed, it is the strongest contender for medical billing software for hospitals and large health centers.
Additional Reading
For more context on how several of these vendors perform as outsourced billing and coding partners, see our guide to the Top 10 Medical Billing and Coding Companies in the US for 2026.
Must-Have Medical Billing Software Features
The medical billing software features that matter most are the ones that directly impact your cash flow, claim accuracy, and staff workload. Here is what to prioritize when evaluating platforms.
Claim Creation, Scrubbing, and Submission
Software that catches errors before submission consistently reduces denial rates. Non-negotiable features in this area include automated claim edits, payer-specific rule checks, and clearinghouse connectivity. Depending on your needs, you may prioritize platforms that support batch submission, real-time status updates, and customizable coding templates.
Eligibility Verification and Prior Authorization Support
Front-end accuracy prevents the most avoidable denials. Real-time eligibility checks at scheduling or check-in confirm coverage, copay amounts, and deductible status before the patient is seen. Prior authorization tools that integrate with payer requirements reduce delays and prevent avoidable denials.
Denial Management and A/R Follow-Up
Even strong claim scrubbing won't eliminate denials—what really matters is how fast your team resolves them. Look for work queues that categorize denials by reason code, payer, and aging bucket. Appeal workflow automation (including letter generation and resubmission tracking) separates strong platforms from basic ones. Clear A/R dashboards with drill-down capability are essential for prioritizing follow-up.
Payment Posting and Patient Billing
Manual payment posting is one of the easiest billing tasks to automate. ERA auto-posting eliminates manual entry for insurance payments. On the patient side, look for automated statements, payment plan options, online portals, and SMS payment links. The goal is to reduce days-to-pay and minimize the volume of accounts sent to collections.
Reporting, Dashboards, and Revenue Analytics
You can't fix what you can't see. Custom dashboards should surface payer performance trends, aging reports, reimbursement patterns, and collection rates—without requiring a data analyst. Exportable reports support internal reviews and external audits.
EHR, PM, and Clearinghouse Integrations
Duplicate data entry is one of the most common sources of billing errors. Bidirectional data flow between your EHR, practice management system, and billing platform eliminates that problem and reduces coding mistakes. Verify that any platform you evaluate integrates cleanly with your existing systems before committing.
HIPAA Compliance, Security, and Access Controls
Role-based access controls, audit trails, encryption at rest and in transit, and automatic logoff are baseline requirements. For a detailed breakdown of what compliance looks like in daily billing workflows, see our guide to HIPAA Compliance in Medical Billing.
Cloud-Based Medical Billing Software vs On-Premise Systems
The market has shifted decisively toward cloud-based medical billing software. But the choice between cloud and on-premise still depends on your organization's size, IT infrastructure, and regulatory requirements.
Below are the main things you need to know to make an informed choice in this important area.
Benefits of Cloud-Based Medical Billing Software
Cloud platforms offer four key medical billing software benefits:
- Remote access from any internet-connected device
- Automatic software updates
- Reduced IT infrastructure costs
- Simpler scalability as your practice grows
Most vendors on our shortlist are cloud-native, reflecting the industry's trend in this direction. For billing teams working across multiple locations—or for organizations using outsourced teams, like Pharmbills—cloud access is essential.
When an On-Premise or Enterprise Setup May Still Make Sense
Large hospital systems with complex IT governance, highly customized environments, or strict data residency requirements may still benefit from on-premise or hybrid medical billing software deployments. Organizations subject to state-level data localization rules, or those running heavily modified EHR configurations that don't translate well to cloud environments, often fall into this category.
Questions to Ask Vendors About Hosting and Data Security
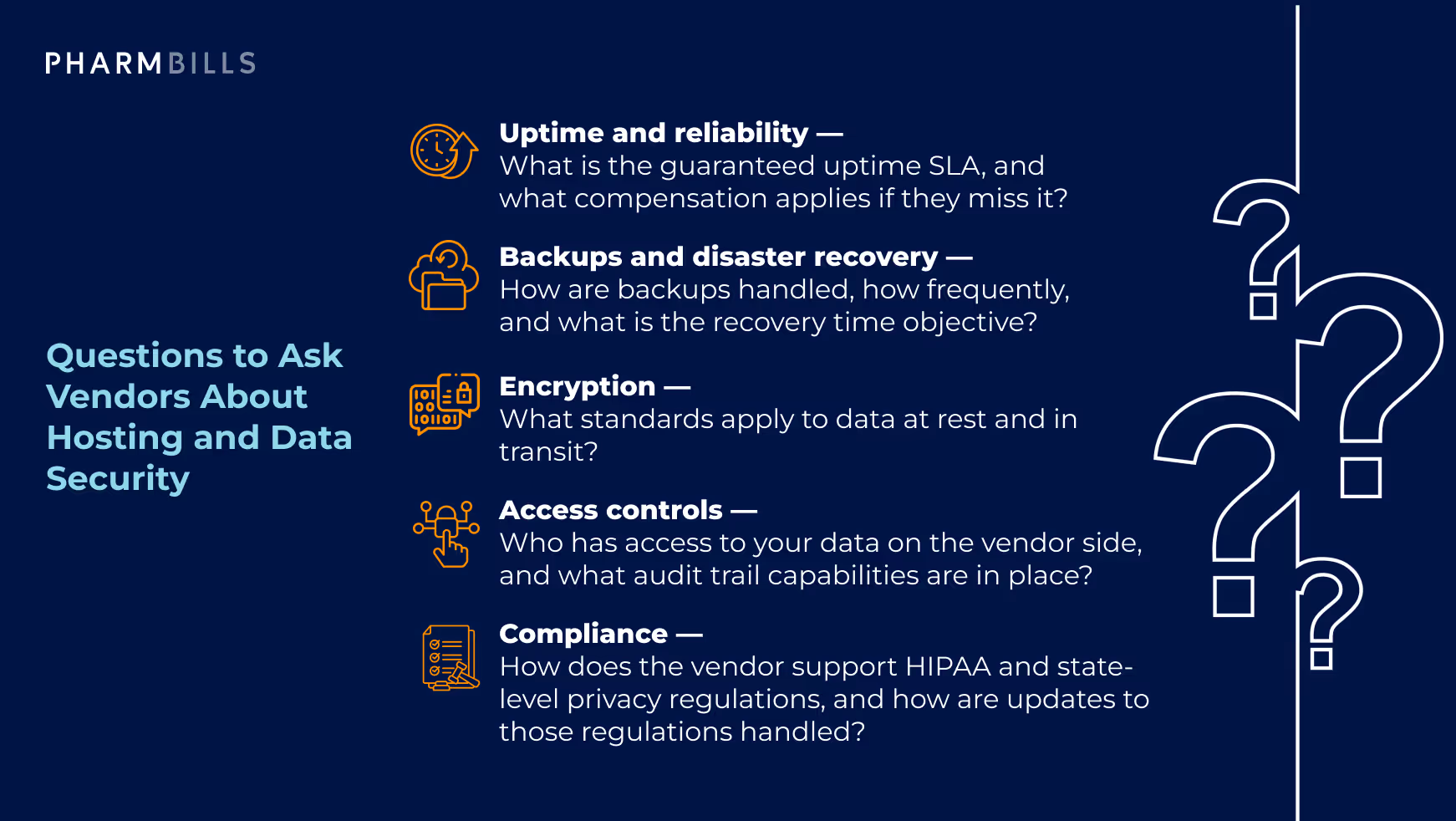
Before committing to any deployment model, ask vendors the following questions:
- Uptime and reliability — What is the guaranteed uptime SLA, and what compensation applies if they miss it?
- Backups and disaster recovery — How are backups handled, how frequently, and what is the recovery time objective?
- Encryption — What standards apply to data at rest and in transit?
- Access controls — Who has access to your data on the vendor side, and what audit trail capabilities are in place?
- Compliance — How does the vendor support HIPAA and state-level privacy regulations, and how are updates to those regulations handled?
Getting clear answers to these questions before signing a contract is far easier than discovering gaps after your data is already on the platform.
Medical Billing Software Pricing: What Buyers Should Expect in 2026
Pricing is one of the most searched and least transparent topics in healthcare software. Most vendors require a sales call before disclosing costs, which makes conducting a proper medical billing software prices comparison difficult.
Common Medical Billing Software Pricing Models
The five main pricing models you will encounter are:
- Per provider per month — The most common structure, ranging from approximately $35 (PracticeSuite) to $449+ (eClinicalWorks), depending on features and vendor.
- Per user per month — Less common, but used by some platforms for administrative-only access.
- Per claim — Typically used by clearinghouses or transaction-based billing platforms.
- Percentage of collections — Usually 4–8% of monthly collections. Aligns incentives, but costs scale with revenue.
- Enterprise custom pricing — Negotiated rates for large organizations with complex requirements.
Understanding which model applies to each vendor on your shortlist is the first step. The next is accounting for the costs that don't appear on the pricing page.
Hidden Costs to Watch For
Unfortunately, there can be a lot of unexpected costs to look out for in medical billing software for clinics and healthcare providers. When conducting a cost comparison, be sure to account for:
- Setup and implementation fees
- Staff training costs
- Clearinghouse transaction fees
- Premium support tiers
- Data migration expenses
- Contract lock-in penalties
Several user reviews we found online cited unexpected add-on charges as a significant frustration.
How to Compare Medical Billing Software Prices Fairly
Sticker price and total cost of ownership are not the same thing. For example, a platform that costs $200 per provider per month but reduces your denial rate by 5% may deliver far more value than a $100 platform that leaves you chasing unpaid claims.
A proper medical billing software prices comparison requires that you evaluate the total cost of ownership across a 12- to 24-month horizon. Factor in:
- Workflow efficiency gains
- Denial rate reduction
- Automation of manual tasks
- Staffing impact.
Be sure to ask vendors for reference customers in your specialty and practice size, and request case studies with documented financial outcomes—not just feature lists.
Practical tip: Build a simple scorecard that weights pricing alongside claims accuracy, support quality, integration fit, and scalability. This prevents the cheapest option from winning by default when a more capable platform might pay for itself within months.
Medical Billing Software Benefits for Providers and Billing Teams

The medical billing software benefits that matter most are the ones that translate directly into financial and operational outcomes. Here is what well-chosen software actually delivers.
Fewer Billing Errors and Cleaner Claims
Automated claim scrubbing catches coding errors, missing modifiers, and payer rule violations before submission. Several of the vendors reviewed in this article demonstrate how automation can directly reduce denial rates.
Faster Reimbursement Cycles
Electronic claim submission, real-time status tracking, and ERA auto-posting eliminate days of manual processing. Organizations that move from paper-based or legacy systems to modern cloud platforms routinely report reductions in days in A/R.
Better Visibility Into Collections and A/R
Custom dashboards and aging reports provide real-time insight into payer performance, outstanding balances, and collection trends. This visibility enables proactive intervention before revenue leakage becomes a pattern.
Lower Administrative Burden
Automated eligibility verification, batch claim submission, and integrated patient payment tools reduce the repetitive manual work that consumes billing staff time. This frees capacity for higher-value tasks like denial resolution and payer negotiations.
More Scalable Billing Operations
Cloud-based platforms grow with your organization. Adding providers, locations, or specialties does not require hardware upgrades or system migrations, which is a critical advantage for practices planning to expand.
More Information
For a comprehensive look at billing best practices that complement your software investment, see our guide on Best Practice Medical Billing in 2026.
How to Choose the Right Medical Billing Software
Selecting the right platform requires a structured evaluation process, not a reaction to the best sales demo. Here is a practical 5-step framework you can follow when conducting a medical billing software comparison.
1. Define Your Billing Workflow and Biggest Pain Points
Start by documenting your current claims volume, denial rates, reporting gaps, manual processes, and payer complexity. A platform that solves your top three pain points will deliver more value than one with the longest feature list.
2. Check Specialty Fit and Integration Requirements
Not every platform supports every specialty well. Verify that your top candidates offer templates, coding support, and payer rules relevant to your clinical focus. Confirm EHR and PM compatibility, clearinghouse connections, and any custom workflow requirements before scheduling a demo.
3. Ask for a Live Demo With Real Billing Scenarios
Request a demo that walks through an actual claim, from eligibility verification through scrubbing, submission, denial handling, and payment posting. Test with your payer mix and specialty codes, not the vendor's pre-built demo script.
4. Compare Support, Onboarding, and Contract Terms
Ask about SLA commitments, implementation timelines, training included versus additional cost, dedicated account management, and cancellation terms. Several platforms in this guide received mixed reviews on post-sale support, so be sure to verify before signing.
5. Use a Shortlist Scorecard Before Buying
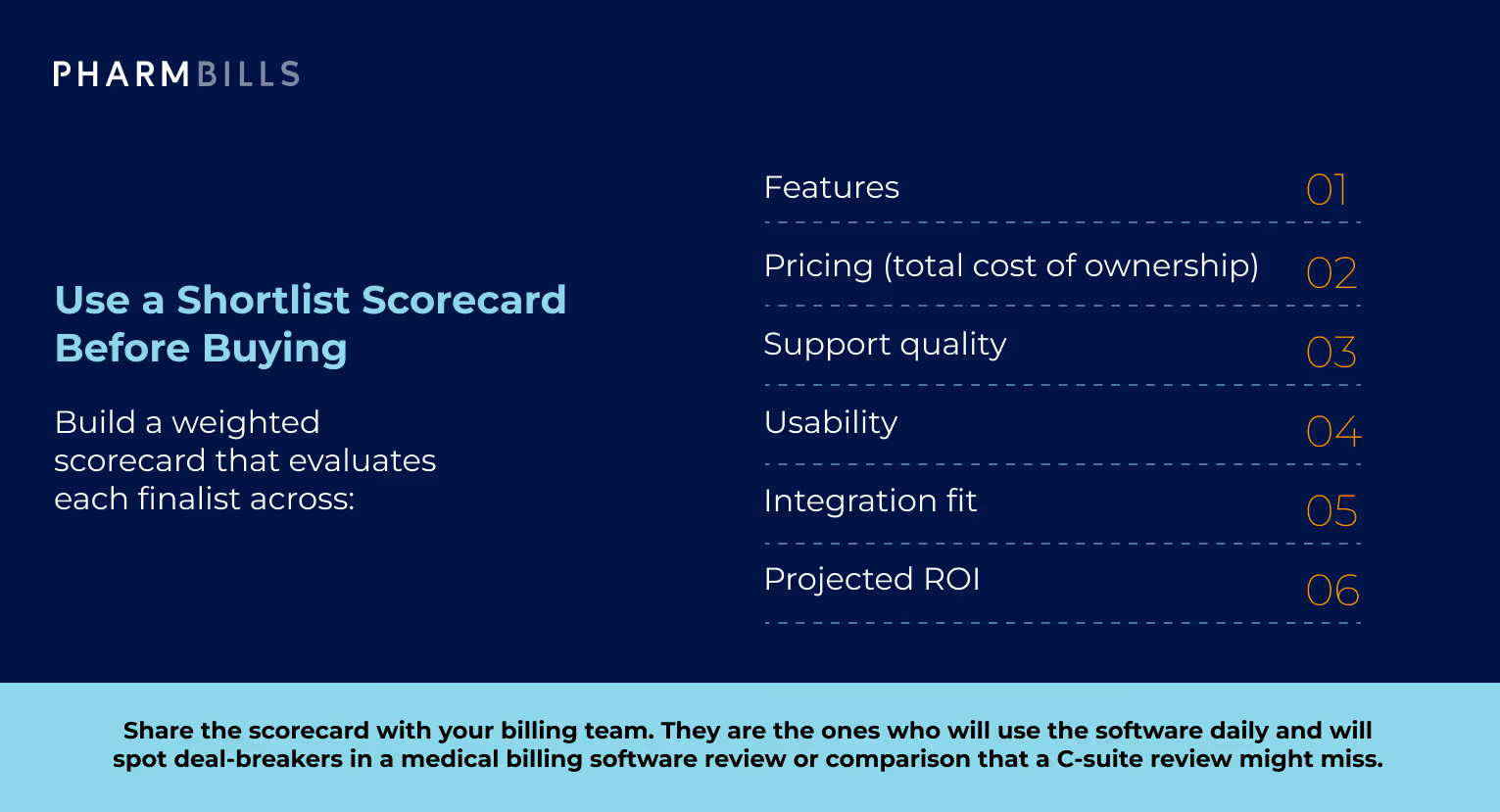
Build a weighted scorecard that evaluates each finalist across:
- Features
- Pricing (total cost of ownership)
- Support quality
- Usability
- Integration fit
- Projected ROI
Share the scorecard with your billing team. They are the ones who will use the software daily and will spot deal-breakers in a medical billing software review or comparison that a C-suite review might miss.
Frequently Asked Questions About Medical Billing Software Comparisons
What is the best online medical billing software in 2026?
There is no single best platform. The right choice depends on your practice size, specialty, payer mix, and budget. This is the reason our medical billing software reviews in this article include details on the best fit by practice type.
How much does medical billing software cost?
Pricing varies widely. Subscription models range from approximately $35 per provider per month (PracticeSuite) to $449+ (eClinicalWorks). Percentage-of-collections models, such as athenahealth's, typically run 4–8%. Always factor in setup fees, training costs, and clearinghouse charges when comparing.
What features should medical billing software include?
At minimum: automated claim scrubbing, real-time eligibility verification, denial management with work queues, ERA auto-posting, patient billing and payment tools, customizable reporting, EHR/PM integration, and HIPAA-compliant security with audit trails.
What is the best medical billing software for small practices?
EZClaim, Tebra, and PracticeSuite are frequently recommended for small practices due to their ease of use, affordable pricing, and focused billing functionality. The right choice depends on whether you want standalone billing (EZClaim) or an all-in-one platform (Tebra, PracticeSuite).
Is cloud-based medical billing software secure?
Yes, when the vendor follows healthcare security standards. Look for encryption at rest and in transit, role-based access controls, audit logging, regular penetration testing, and SOC 2 or HITRUST certification. All cloud-based platforms reviewed in this guide support HIPAA compliance.
What is the difference between medical billing software and practice management software?
Medical billing software focuses specifically on claims creation, submission, tracking, denial management, and payment posting. Practice management software is broader, covering scheduling, patient registration, reporting, and front-office workflows. Many modern platforms combine both into a single suite.
Can medical billing companies use the same software as healthcare providers?
Yes. Several platforms, including PracticeSuite, EZClaim, and CollaborateMD, are specifically designed to support third-party billing companies with multi-practice dashboards, batch processing tools, and per-client reporting. This is relevant if you are conducting a medical billing software for third party billing companies prices comparison.
Summing Up: Online Medical Billing Software Comparison
There is no universal "best" medical billing software. The right platform depends on your practice size, claim complexity, specialty, integration requirements, reporting needs, and pricing tolerance. What every organization has in common is the need for clean claims, fast reimbursements, visible A/R, and manageable costs.
When conducting a medical billing software comparison, use the comparison table and reviews in this guide to build a shortlist, then request demos with real billing scenarios from your specialty and payer mix. During the demo, apply the five-step structured checklist we provided under "How to Choose the Right Medical Billing Software" so you can make an objective assessment based on real-world data—not a polished sales presentation.
Finally, be mindful that choosing the right software is only half the equation. The other half is having skilled people to operate it. If you already have billing software and need dedicated, experienced professionals to run it at maximum efficiency, reach out to Pharmbills today to discuss how our outsourced billing teams can integrate directly into your existing workflow.





![Strategies for Healthcare Revenue Cycle Optimization [2026]](https://cdn.prod.website-files.com/63d9425d235def15b898f020/662b859ab4ed0e9043c16de9_21826165.avif)

