Extreme administrative pressure has become the baseline for many medical billing teams rather than the exception. At the top of the list of issues contributing to this problem are payer rules that shift constantly, denial rates that keep climbing, and a consistent shortfall in the number of certified coders and experienced billers needed to keep up with daily operations.
Artificial intelligence has become part of the response, with organizations investing roughly $1.4 billion in healthcare AI solutions in 2025 (nearly triple the prior year). However, while AI in medical billing is a genuinely useful tool in some operations, its full value can only be realized when it is applied to the right problems, with the right oversight.
This article walks through what AI medical billing actually does today, where it adds value, where it falls short, and what healthcare organizations should look for when evaluating solutions.
Related Services
For broader context on how Pharmbills supports healthcare organizations, read more about our Medical Billing Services.
What AI in Medical Billing Actually Means
Medical billing AI is not a single product. It is a category that covers several distinct technologies, and treating them as interchangeable can lead to bad purchasing decisions and unrealistic expectations.
Most billing operations today involve a blend of capabilities that get marketed under the AI umbrella. The four main capabilities are described below. Although, as we'll see, not all of them are strictly classed as AI.

1. Rules-Based Automation
Rules-based automation uses deterministic "if-this-then-that" logic to execute predefined actions. The most common form in billing operations is robotic process automation (RPA) — software bots that mimic human actions across systems.
While not technically AI, the underlying mechanism of rules-based automation is reliable for repetitive, predictable tasks such as eligibility pings, claim status checks, and routing standardized claims. It does not learn or adapt. But for high-volume routine work, that is a feature, not a limitation.
2. Machine Learning and Predictive Tools
Machine learning (ML) algorithms ingest historical claims data to spot patterns. Many of these tools rely on natural language processing (NLP), a related AI technique that lets software read and interpret unstructured text like physician notes or remittance advice.
Predictive analytics — a subset of ML — forecasts outcomes such as the likelihood of a denial before a claim is even submitted, allowing teams to intercept problems early. The accuracy of these tools improves as they ingest more data, which means deployments tend to deliver stronger results 6 to 12 months in than they do at launch.
3. Generative AI
Generative AI refers to deep learning models that produce new text. These models are often combined with NLP to read source documents before drafting output.
In medical billing, generative AI is most often used to draft appeal letters, summarize complex payer policy changes, or translate clinical jargon into plain language for patient statements. Output quality varies significantly with prompt design and source data, which is why generative AI works best as a drafting assistant rather than a final authority.
4. Workflow Intelligence and Prioritization
Less flashy but operationally important workflow intelligence and prioritization tools use AI to rank work queues so staff focus on the highest-value tasks first (for example, surfacing aging denials with strong appeal potential before lower-impact items). The financial impact often comes less from automation itself and more from making sure scarce coder and biller hours land on the work that actually moves revenue.
It’s important to note that most medical billing teams are not replacing the entire process with AI. They are layering specific tools onto specific workflows, while keeping experienced people in charge of judgment-heavy work.
Additional Insights
For a clearer view of where AI could be used across all billing and coding workflows, see our article on Medical Coding vs. Medical Billing: Understanding the Core Differences.
Where AI Is Used Across the Medical Billing Workflow
AI shows up at almost every stage of the revenue cycle, but the depth of automation varies. The table below shows where AI systems in medical billing and coding are currently doing meaningful work — and where human review is still required.
AI Use Cases Across Billing Workflows
Front-end errors alone account for roughly 46% of all eventual claim denials, which is why integrating AI into intake-stage workflows tends to be an initial priority area for healthcare organizations.
The Biggest Operational Problems AI in Medical Billing Can Help Reduce
Most billing teams are implementing AI tools to get relief from a small set of operational problems that have been getting worse for years. These challenges can be grouped into several broad categories that are described below.
Manual Repetitive Work and Data-Entry Errors
A large share of billing time goes to tasks that are predictable, high-volume, and prone to small mistakes (eligibility verifications, claim status checks, demographic entry, etc). RPA and ML-driven automated billing tools can autonomously handle the routine version of this work and flag exceptions for human review, cutting down on both labor hours and the errors that come with fatigue.
Missed Billing Opportunities and Slow Follow-Up
Charges get missed, denials sit in queues, and around 60% of denied claims are never even resubmitted — which translates to billions in lost revenue annually across the industry. AI tools that scan documentation for unbilled services and prioritize aging denials can help close these gaps, especially for teams that are short-staffed.
Fragmented Workflows and Limited Capacity
Many billing teams work across several systems that do not talk to each other cleanly (EHR, practice management, clearinghouse, and payer portals). AI cannot fix integration problems on its own, but workflow intelligence layers can route work accurately and reduce the number of handoffs each claim requires.
The pattern in the points above is consistent: AI delivers most when it absorbs the routine, surfaces the overlooked, and connects what is already fragmented.
Real Benefits of AI in Medical Billing
The benefits of AI medical billing tools are real, but they are also highly specific. The strongest results come from targeted deployments tied to measurable goals, not from broad "transformation" initiatives. In practice, these benefits cluster around five key areas.
Faster Workflow Execution
AI cuts the number of manual touches per claim. Tasks that previously required a coder to open a chart, review documentation, and key in codes can now happen in a fraction of the time for routine encounters. Hospitals using RPA for repetitive administrative tasks have reported saving between 1,500 and 3,000 staff hours annually.
Better Billing Accuracy and Cleaner Claims
AI for medical billing does not guarantee perfection, but it does add a validation layer. Before claims even leave the building, anomaly detection can catch issues like:
- Missing modifiers
- Mismatched demographics
- Bundled-code conflicts
Facilities deploying RPA and AI-driven validation often see meaningful improvements in clean claim rates, though the size of the gain depends on baseline data quality.
Smarter Denial Management
Predictive AI assigns each claim a probability-of-denial score, allowing teams to intervene before submission. Kaiser Permanente's six-month pilot of an AI-driven denial management platform reduced initial denial rates by 17%, by flagging eligibility mismatches and missing documentation. On the back end, generative AI can draft appeal packages roughly three times faster than manual processes.
Better Visibility Into Revenue Cycle Performance
Dashboards built on AI-surfaced patterns help leaders see what is happening across payers, specialties, and individual staff workloads. A specific commercial payer underpaying a single CPT code by 3% across hundreds of locations would typically slip past human auditors. However, when properly tuned, AI would almost certainly identify an RCM discrepancy like this.
Improved Staff Efficiency (Not Just Lower Headcount)
This is perhaps one of the most important points about medical billing AI. The strongest deployments do not aim to shrink the billing team. They aim to redirect existing staff toward higher-value work — appeals, payer strategy, complex specialty coding — while AI absorbs the repetitive load. That shift is where the real efficiency gain lives. Not in fewer people, but in better-deployed ones.
The common thread in all of the examples above is that AI delivers best results when it is paired with thoughtful human-centred workflow design.
What AI in Medical Billing Cannot Reliably Do on Its Own
This is the section that most vendor websites skip. AI medical billing tools are powerful, but they have specific failure modes that buyers need to understand before deployment. Put another way, AI can accelerate billing work, but unsupervised automation creates downstream errors that are often harder to catch than the manual mistakes it replaced.

Here are the main capabilities that AI consistently struggles with:
- Reading clinical context accurately. Generative AI can produce plausible-sounding output that is factually wrong. A 2025 study published in NPJ Digital Medicine found that AI ambient scribes frequently produced "hallucinations," including fabricated diagnoses and physical exam findings that never occurred.
- Handling specialty-specific or payer-specific nuance. Oncology coding, transplant medicine, and complex cardiology cases involve qualitative judgments that current models do not handle well. Payer-specific rules also shift in ways that generic AI tools miss, particularly for Medicare Advantage plans, where coverage criteria and reimbursement logic change frequently.
- Recovering from poor input quality. AI is only as good as the data it ingests. Incomplete documentation, fragmented systems, and inconsistent coding habits upstream all degrade AI output downstream.
- Operating without supervision in high-stakes scenarios. Generative AI in particular should not be treated as an autonomous authority. The American Medical Association has explicitly called for human review on prior authorization decisions after reports that one major payer denied over 300,000 claims using an AI process averaging 1.2 seconds per case.
The takeaway from all four points is straightforward: AI is a tool, not a decision-maker. Treating it as the latter can leave organizations exposed to significant risk.
Risks, Compliance, and Oversight Considerations
Beyond capability limits, medical billing AI introduces a set of risks that buyers need to evaluate seriously. These are not theoretical concerns — they are the issues mature billing operations are actively managing as digital transformation in healthcare billing accelerates.
The risks cluster around data protection, governance, output quality, and implementation. Mature buyers evaluating medical billing and AI need to weigh each separately, since each calls for a different kind of response.
Data Privacy and HIPAA-Related Considerations
Any AI system handling claims is also handling electronic Protected Health Information (ePHI). The HHS Office for Civil Rights proposed a major update to the HIPAA Security Rule in January 2025, specifically to address AI, cybersecurity, and ePHI. In short, organizations now need to confirm vendor encryption standards, enforce least-privilege access, and guard against "shadow AI" — staff pasting patient information into public chatbots to get work done faster.
Governance, Transparency, and Human Oversight
Healthcare organizations are increasingly aligning their AI deployments with the NIST AI Risk Management Framework and demanding explainability from vendors. Black-box algorithms that cannot explain their recommendations are now widely rejected for billing use. Strong governance also requires documented human-in-the-loop checkpoints at high-stakes decision points, particularly around coding and prior authorization.
Bias, False Confidence, and Poor Decision Quality
AI outputs can sound convincing while still being wrong. Researchers have found significantly higher error rates when AI scribes process data from Black patients, indicating a pattern of algorithmic bias with direct implications for billing integrity. Confident-sounding AI outputs need source grounding. In other words, the system should be able to point to the exact documentation that justifies any code or recommendation.
Integration Risk and Workflow Disruption
Bad implementation can slow teams down rather than helping them. AI tools that do not integrate cleanly with the EHR, that require constant context-switching, or that produce more alerts than staff can act on tend to get abandoned within months. The strongest deployments invest heavily in workflow design before turning anything on, treating the technology as the last piece of the puzzle rather than the first.
Deep Dive
For a more detailed look at HIPAA obligations specific to billing operations, see our guide on HIPAA Compliance in Medical Billing.
AI in Medical Billing vs Human Billing Teams
The most useful framing for AI systems in medical billing and coding is not "AI vs humans." It is "what does each do best, and how do they combine?" The comparison below outlines where each approach has structural strengths.
AI Compared to Human Billing Teams
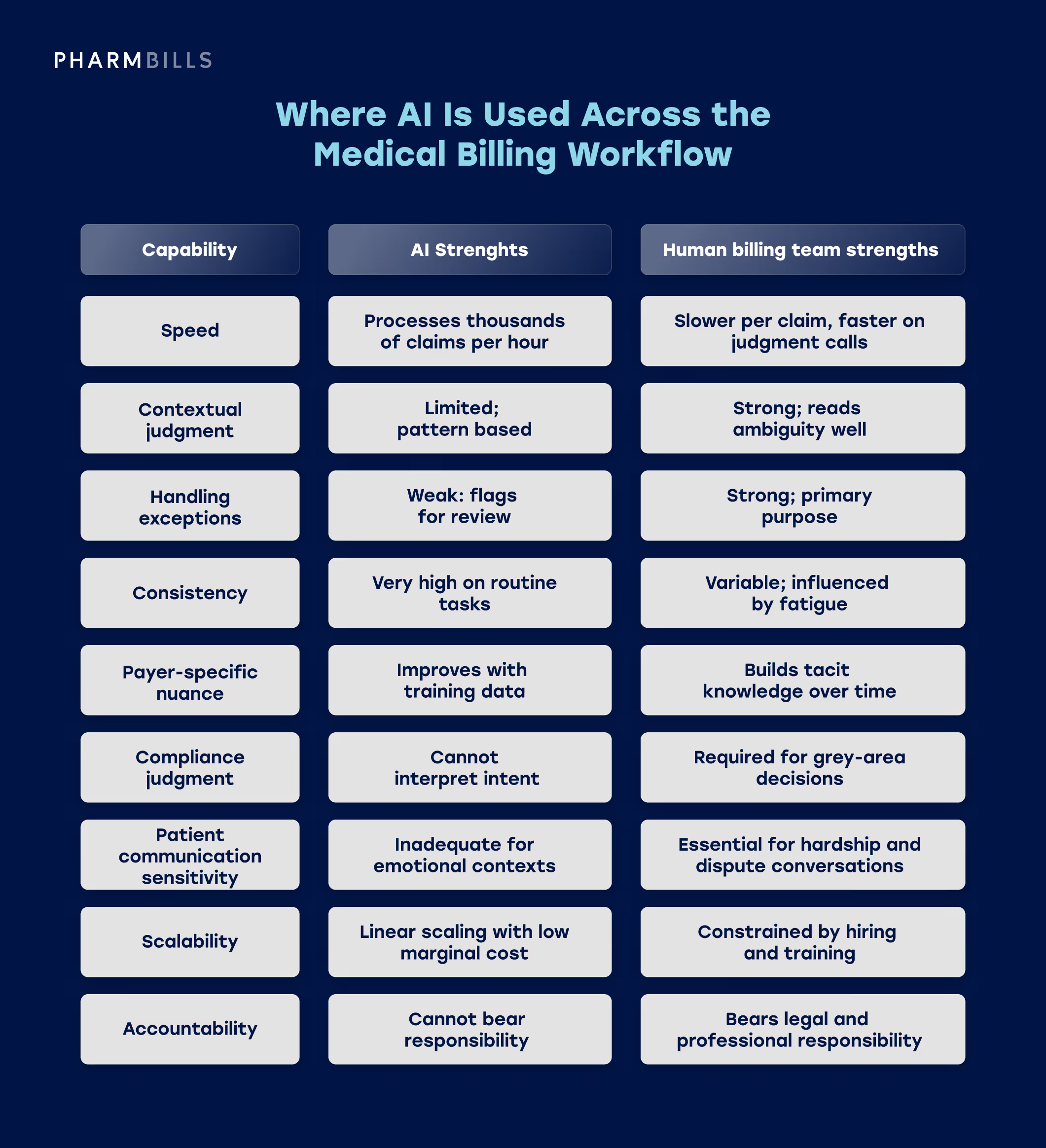
The strongest operating model at present is AI-assisted human billing, where AI handles volume and people handle judgment.
Organizations that try to skip the human layer tend to discover the hard way that the cost of automated billing mistakes exceeds the savings from automated work.
Is AI Replacing Medical Billing Jobs?
Here’s one of the most common questions healthcare leaders are asking today: “Is medical coding and billing being taken over by AI?”
The short answer is no. But the nature of billing work is changing significantly. Routine coding, basic claim status checks, and standardized eligibility verification are increasingly handled by AI-enhanced medical coding tools, with human staff handling higher-order skills.
Here are the main factors keeping humans firmly in the picture when it comes to healthcare billing:
- Complex specialties still require trained people. Oncology, cardiology, transplant medicine, and similar high-acuity areas involve clinical and coding judgment that current AI cannot reliably replicate. The volume of edge cases in these specialties is high enough that automation tends to create more review work than it removes.
- Compliance and audit defense need accountability. AI cannot bear legal responsibility for a billing decision. Coders, billers, and revenue cycle leaders still do. This means human review remains the final safeguard against the federal compliance exposure that comes with miscoded or misjustified claims.
- Payer disputes require strategy. Generative AI can draft an appeal letter, but the framing, evidence selection, and escalation strategy remain human work. This is especially true for high-dollar claims, where a single appeal can swing six or seven figures and the payer is using their own AI to push back.
- Patient communication is irreducibly human. Sensitive conversations about balances, hardship, and disputes do not translate well to chatbots. This becomes more important as patients themselves now use AI to scrutinize their bills, which means billing teams are increasingly fielding sophisticated, AI-prepared questions from the people they serve.
Across all points, the pattern is the same: billing professionals should expect their roles to shift toward review, exception handling, and judgment work — and organizations should evaluate vendors on whether they support that shift or try to bypass it.
Financial Impact: Where AI Can Support ROI in Billing Operations
The financial case for AI-driven revenue management in medical billing is real, but it depends heavily on how the technology is deployed.
Healthcare organizations that report measurable returns typically see them within 12 to 24 months, and the financial impact tends to show up in direct efficiency gains and revenue recovery. Both depend on a factor that often goes underdiscussed: how mature the underlying workflow is before AI gets layered on top.
Direct Efficiency Gains
The most immediate financial impact of AI in medical billing comes from labor reallocation. When AI absorbs routine claims validation and rework, billing staff can focus on the work that actually moves revenue — and that shift shows up in the numbers.
AdventHealth's deployment of RPA for claims validation, for example, shortened denial rework cycles by nearly 30% without increasing headcount. Across the industry, strategic AI integration has been associated with meaningful reductions in days in accounts receivable, which directly accelerates cash flow.
Revenue Protection Opportunities
The bigger financial story is often revenue recovery rather than cost reduction. AI tools that surface unbilled services, identify systemic underpayments, and prioritize aging denials tend to find money that would otherwise stay lost.
One 200-physician orthopedics group using AI-powered contract management recovered $10.3 million in hidden underpayments from just seven commercial payers. Given that healthcare providers face hundreds of billions in denied claims annually — most of which is never recovered — even modest improvements in this area translate to meaningful financial returns.
Why ROI Depends on Workflow Maturity
There is no automatic payoff with medical billing AI. Organizations with messy data, fragmented systems, or undertrained staff frequently see worse outcomes after deployment, not better.
Financial benefits depend on data quality, process discipline, and human oversight. AI generally amplifies whatever is already there, with mature operations getting more out of the same tools than chaotic ones do.
In summary, AI does not generate financial returns on its own. It accelerates and protects returns that the underlying operation is already capable of producing.
Pricing Context
For a clearer picture of how billing service costs are structured and how AI factors into pricing, see our guide on Medical Billing Rates & Fees: How Much Does Medical Billing Service Cost in 2026?.
How Healthcare Organizations Should Evaluate AI Billing Solutions
Before signing a contract for healthcare AI solutions in billing operations, healthcare leaders should work through a structured evaluation.

The questions below come from procurement frameworks used by industry analysts and are designed to separate viable enterprise solutions from marketing-driven ones. Treat them as a working checklist for vendor conversations. Any vendor unwilling or unable to answer these directly is signalling something important about the maturity of their product.
- Does it integrate with current systems? Seamless HL7 or API integration with the existing EHR is a baseline requirement. Tools that require constant context-switching tend to be abandoned within months.
- What does it automate vs. recommend? Be precise. Some tools execute end-to-end; others surface suggestions for staff to act on. Both can be valuable, but they require very different governance structures.
- Is there human review built in? Workflows should include human-in-the-loop checkpoints at high-stakes decision points. Vendors that resist these checkpoints are usually selling a level of automation the organization is not actually ready to govern.
- How is data protected? Vendors should provide updated Business Associate Agreements that explicitly cover AI training, inference, and subprocessing. Encryption standards, access controls, and audit logging should all be documented.
- How are errors surfaced and corrected? Strong systems explain their reasoning and link outputs back to source documentation. If an AI cannot show why it suggested a specific code, it is not ready for compliance-sensitive work.
- Can the vendor explain where AI is used and where it is not? Marketing teams blur this line. Procurement teams should demand clarity.
- Does the solution improve workflows or add another layer of software? A new tool that does not reduce overall complexity is a problem, not a solution.
- Who remains accountable for outcomes? Accountability cannot transfer to the vendor. The healthcare organization owns billing decisions and their consequences — the vendor relationship needs to reflect that reality.
One last filter: weight long-term track record over recent marketing. Vendors that have sustained strong client outcomes across multiple years are usually the safer bet, even when newer entrants look more exciting on paper.
Vendor Landscape
For a curated overview of established providers in the space, see our analysis of the Top 10 Medical Billing and Coding Companies in the US for 2026.
When Outsourced Medical Billing Makes More Sense Than Software-Only Automation
Software alone does not solve workflow problems. This is where many AI-first deployments stall: the technology arrives, but the people, processes, and payer expertise needed to use it optimally do not. The conversation about medical billing and AI tends to skip over this point, which is part of why so many implementations underperform.
For many healthcare providers, the most practical path is a combination of technology and operational support, not a pure software purchase. Outsourced billing teams like Pharmbills can bring three things that software cannot:
- Experienced billing professionals - who understand specialty-specific coding, payer behavior, and the realistic limits of automation.
- Process discipline and ownership - someone who is accountable for the workflow end-to-end, not just the tools that support it.
- Continuous payer expertise - knowledge of how rules are shifting across commercial payers, Medicare Advantage plans, and Medicaid programs, which AI tools alone cannot keep up with.
The strongest model for many organizations is operational support paired with intelligent tools, rather than buying software and hoping internal teams can build the missing capability. This is particularly true for smaller practices and specialty groups, where the in-house resources required to properly deploy and govern AI often exceed the savings the tools were supposed to deliver.
More Information
For a closer look at evaluating outsourcing partners, see our guide on How to Choose the Right Medical Billing Outstaffing Company.
AI Medical Billing: Final Thoughts
AI for medical billing is real and increasingly capable. But its value depends on thoughtful deployment, not on the technology itself. The organizations getting the most out of AI are treating it as one component of a stronger billing strategy — paired with experienced staff, clear governance, mature processes, and realistic expectations.
In contrast, buying software and hoping it solves underlying operational problems tends to produce the worst outcomes. In most cases, AI amplifies whatever is already in place. Strong operations get stronger; weak ones get faster at making the same mistakes.
For healthcare providers planning their billing strategy, the question is not whether to use AI in medical billing. It is how to use AI responsibly, with the right oversight, and within the right operational model.
If you are evaluating how AI fits into your billing operations, get in touch with our HIPAA-compliant billing team. We can walk you through where automation makes sense for your specific workflow, and where experienced human oversight will add the most value.





![Strategies for Healthcare Revenue Cycle Optimization [2026]](https://cdn.prod.website-files.com/63d9425d235def15b898f020/662b859ab4ed0e9043c16de9_21826165.avif)

