Every year, US healthcare providers leave billions of dollars on the table through avoidable claim denials, slow follow-up, and billing errors. In 2026, with compliance expectations tightening and payers deploying AI to automate claim reviews, it’s never been more important to select the right billing partner.
When healthcare providers thoughtfully choose the best medical billing company for their needs, claims are cleaner, payments are faster, denials reduce, and the whole revenue cycle runs smoothly without constant firefighting. Getting it wrong means the opposite: mounting A/R, compliance exposure, and a painful vendor transition down the road.
This guide gives you everything you need to confidently choose the right medical billing company. Inside, you’ll find a 13-step evaluation framework, a full vendor interview question bank, a weighted scorecard, contract negotiation guidance, and a final checklist to keep your process on track.
Related Services
Explore how Pharmbills supports healthcare organizations across the full billing lifecycle with expert Medical Billing Services.
Step 1 — Define Your Practice Needs (Before You Talk to Vendors)

The most common mistake when evaluating medical billing services for healthcare providers is starting with vendor conversations before you've documented what you actually need. Spend time on this task first, as it will sharpen every conversation that follows.
Before reaching out to any medical billing vendors, clarify and document your practice needs in the following areas:
- Specialty and care setting - Primary care, behavioral health, orthopedics, long-term care facilities, and ambulatory surgery all have different coding complexity and payer mix dynamics. Ensure that you’re clear on these so you can clarify if the vendor has expertise in your area.
- Monthly claim volume - The number and value of claims your organization has each month affects which medical billing companies might be the right fit and which pricing models make sense. You’ll need to know these numbers before negotiating any contracts.
- Payer mix - Government payers (Medicare, Medicaid) have different compliance requirements than commercial insurers. A high Medicaid volume, for example, demands a medical billing vendor with deep familiarity with state-specific rules.
- Current pain points - Is your revenue cycle struggling with high denial rates, slow accounts receivable follow-up, posting delays, or credentialing backlogs? Naming problems precisely helps you evaluate whether a vendor can actually solve it.
- In-house staff gaps - Are you looking at outsourced medical billing services to replace a function entirely, or to supplement your existing team? In most cases, the best medical billing company will be the one that can address all of your talent gaps.
- EHR and practice management system - Know your current tech stack before entering any tech compatibility conversation. EHR integration for medical billing partners is vital, as the vendor must be able to work within your existing systems.
Size is a final consideration to take into account when evaluating medical billing companies. Vendors that excel for a solo practice with 300 claims per month are often a poor fit for a 20-provider multi-specialty group with complex payer contracts. Defining your profile upfront prevents that mismatch.
Additional Information
For more on how choosing the best medical billing outsourcing company can improve revenue and operations, see Reasons to Hire a Medical Billing Specialist: Key Benefits.
Step 2 — Decide the Scope: Billing-Only vs Full RCM Outsourcing
Not all healthcare business process outsourcing engagements look the same. Medical billing outsourcing for clinics and larger providers can range from a narrow billing-only arrangement to a fully managed revenue cycle operation. Getting this scope decision right before vendor conversations saves significant time.
Use this table to clarify the scope of medical billing support required for your organization.
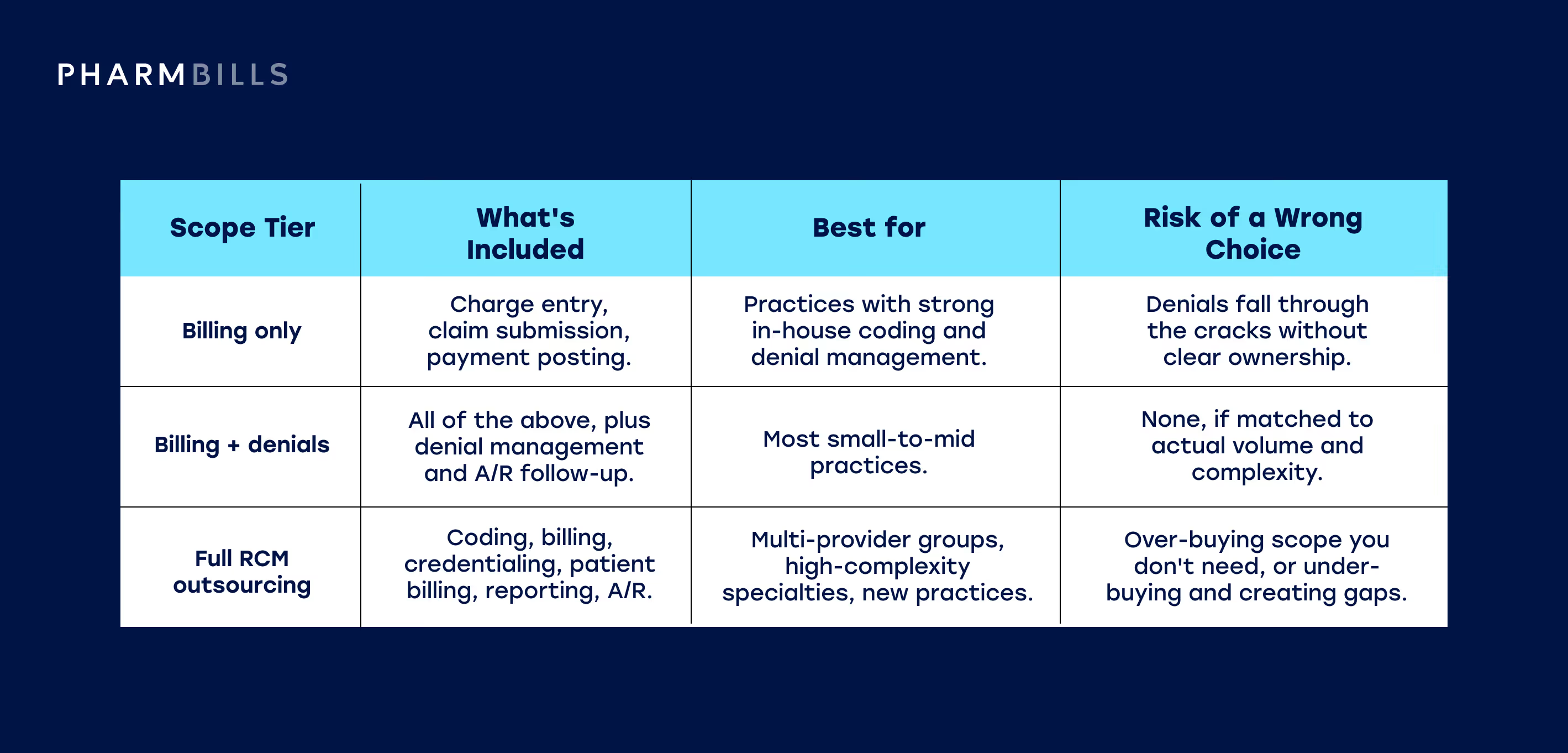
Here are a few quick decision cues to get you started:
- If your denial rate is above 8% or your days in A/R consistently exceed 40, you likely need more than billing-only.
- If you lack certified coders in-house, scope in coding support from day one.
- If you're launching a new practice or expanding locations, credentialing and enrollment should be part of the conversation.
Once you’re clear on scope, the next step for choosing the best medical billing company is to evaluate compliance and security.
Step 3 — Must-Have Compliance and Security in 2026 (Non-Negotiables)
Details about security and compliance are non-negotiable questions to ask a medical billing company. Any vendor operating in 2026 must treat HIPAA not as a checkbox, but as a core operating discipline.
Here's what to verify about medical billing compliance (HIPAA, BAA, etc) in plain English before you sign anything:
- Business Associate Agreement (BAA) - A current BAA is required by law before any medical billing service can access protected health information (PHI). If a vendor hesitates on the BAA, stop the conversation.
- Access controls - You must know who inside the vendor's organization can access your patient data? In particular, ask if access controls are role-based and documented?
- Audit trails - Can the vendor show you logs of who accessed what data, made changes, and when?
- Data encryption - PHI should be encrypted both in transit and at rest. Ensure that you get specifics, not reassurances.
- Incident response plan - What happens if there's a breach of PHI or confidential information? Who notifies you, in what timeframe, and what steps follow?
- Subcontractors - Many billing vendors use subcontractors for specific functions. Those subcontractors also need to be HIPAA-compliant and covered by a BAA.
When talking with medical billing companies about security and compliance, ask for written proof, not verbal assurances. Relevant documentation includes published security policies, third-party certifications (SOC 2, HITRUST), completed security questionnaires, and recent audit results. Any vendor that can't produce these on request may be a compliance risk.
Further Insights
For a thorough overview of what HIPAA means for your billing operations, see HIPAA Compliance in Medical Billing: A Comprehensive Guide.
Step 4 — Specialty Experience and Coding Quality (Where Revenue Gets Won or Burned)
Coding is where revenue gets won or lost. So if you really want to select the right vendor, generic experience is not enough. The best medical billing company for coding in your specialty will have deep familiarity with the CPT codes, ICD-10 pathways, and payer-specific documentation requirements that apply to your care setting.
When evaluating a company’s coding quality, ask for:
- Specialty-specific client references - Not just "we work with physician practices." Ask for references from practices with your specialty and a similar payer mix.
- Examples of coding complexity handled - Behavioral health, cardiology, radiology, and orthopedics each carry specific coding challenges. Ask how the vendor manages upcoding risk, bundling edits, and modifier usage in your specialty.
- Coder certifications - In 2026, AAPC certified coders (CPC, CRC, COC) and AHIMA certified coders (RHIA, RHIT, CCS) remain the recognized standard. Ask what percentage of the coding team holds active certifications and what continuing education is required.
- Coding QA process - What internal audit process is in place? How often are charts reviewed for accuracy, and how are errors tracked and corrected?
Please note that a coding accuracy rate below 95% is a red flag. Be sure to ask vendors for documented benchmarks, not estimates.
Step 5 — Technology Fit: EHR/PM Integration, Clearinghouse, and Automation
Technology compatibility is a key component of medical billing company evaluation criteria, as a poor tech fit can create more administrative burden than it solves.
Here's what to look at when deciding on the best medical billing company:
- EHR and practice management software integration - Can the vendor work within your existing system? Any requirement to migrate your EHR should be weighed against the full cost and disruption of that transition.
- Clearinghouse relationships - Which clearinghouses does the vendor use, and do those clearinghouses have direct connections with your primary payers?
- Claim scrubbing software - Does the company apply automated edits before claims submission to catch errors that would generate denials? Ask for denial prevention rates as evidence this works.
- Eligibility verification - Is real-time eligibility checking integrated into the workflow before every appointment?
- Denial management process - How are denials tracked, assigned, and escalated? Is there a system of record, or is it managed via spreadsheets?
- Patient payment tools - Does the vendor support patient statements, payment plans, and online payment portals?
One of the best ways to gather the information above is through a demo. Ideally, ask for a live demo that shows claim scrubbing software in action, a denial workflow from identification through resolution, and a reporting dashboard with real KPI data.
Step 6 — Performance Metrics That Actually Matter (KPIs + Reporting)
Transparent, consistent reporting is one of the clearest differentiators between a strong medical billing services partner and a weak one. Before signing a contract, agree on exactly which KPIs will be tracked, how they're defined, and how often you'll receive reports.
The key metrics for choosing the best medical billing company are:
- Clean claim rate - Percentage of claims accepted on first submission. Best-in-class is consistently above 95%.
- First-pass resolution rate (FPRR) - Percentage of claims paid on the first submission without manual intervention. Aim for 90%+.
- Denial rate - Percentage of submitted claims denied by the payer. Industry denial rate benchmark averages hover around 5–10%. Anything above 10% warrants caution.
- Days in accounts receivable (days in A/R) - The average number of days between service delivery and payment. Below 35 days is a strong benchmark for most specialties.
- Net collection rate - Percentage of collectible revenue actually collected. Below 95% indicates money is being left on the table.
- Aging buckets - What percentage of the company’s A/R is over 90 days? Over 120 days?
- Lag time - How quickly are charges entered after the date of service?
It’s recommended to require reporting on a defined cadence (weekly for the first 90 days is reasonable; monthly thereafter). Insisting on dashboard access is also wise, so you can review data between formal reports. Any vendor that can't define these KPIs precisely or refuses dashboard access should be treated with caution.
Step 7 — Pricing Models in 2026 (and How to Spot ‘Cheap’ That's Expensive)
There is no single correct pricing model for outsourced medical billing, but there are several ways to overpay without realizing it. Understanding your options and what each one actually costs in practice is the first step to making a fair comparison.
Here are the most common medical billing pricing models:
- Percentage of collections - Typically 3–8% of collected revenue. Vendor incentives align with your revenue. Medical billing pricing on a percentage of collections works well if your volume is stable and collections are strong.
- Per-claim (flat fee) - A fixed fee per claim submitted, regardless of outcome. Per-claim pricing is predictable, but doesn't incentivize denial follow-up the same way.
- Flat monthly retainer - A fixed monthly fee. Flat monthly retainers are simple to budget, but can result in overpaying if claim volume fluctuates.
- Hybrid - A base retainer plus a percentage or per-claim fee. Hybrid arrangements are common for larger or more complex engagements, and are offered by some of the best medical billing companies in the USA.
Hidden Fees in Outsourced Medical Billing
The list above covers standard fees that are relatively easy to calculate. But there are also often additional ancillary that are easy to overlook, such as:

Calculating the True Cost
Here’s a simple "true cost" formula when evaluating the best medical billing outsourcing company for your needs.
Take the quoted rate, add all ancillary fees, then divide by your average monthly collections. That gives you an effective cost percentage that's comparable across vendors.
More Details
For a comprehensive breakdown of what medical billing services typically cost in 2026, see Medical Billing Rates & Fees: How Much Does Medical Billing Service Cost in 2026?
Step 8 — Contract Terms and SLA: What to Negotiate (and What to Refuse)
A medical billing contract service level agreement (SLA) protects both parties, but the standard terms often favor the vendor. Here are 10 vital questions to ask before signing anything:
- What is the minimum contract term, and what are the renewal conditions?
- What are the termination notice requirements, and is there an early termination fee?
- Who owns the billing data, and how is it transferred if the relationship ends?
- What KPIs are defined in the SLA, and what happens if they're missed?
- What is the response time commitment for denial appeals and A/R follow-up?
- How is compliance liability handled if a billing error results in an audit?
- What is the process for adding or removing services mid-contract?
- Are subcontractors used, and are they covered by HIPAA BAAs?
- What constitutes a material breach, and what remedies are available?
- What does the off-boarding process look like, including data handoff and transition support?
If you see an evergreen renewal clause with no notice window, a termination fee exceeding one month's billing, or vague SLA language with no defined remedies, push back or escalate to legal review. These terms are negotiable more often than vendors suggest.
Step 9 — Due Diligence: Reputation, References, and Proof
Vendor marketing materials tell you what a company wants you to believe, while references, performance data, and customer reviews tell you what's actually true. The best medical billing company in USA for your needs is one that can back its claims with documented results and has a good reputation in the community.
Finding Reviews and Assessing Reputation
Here are some sources for finding reviews on a company and gaguing its reputation:
- Google Reviews, Capterra, G2, and KLAS (for larger vendors) offer independent user feedback.
- LinkedIn can surface former employees and clients whose experience may be worth a direct conversation.
- CMS exclusion lists enable you to verify that the vendor is not on the OIG exclusion database.
What to Ask In Reference Calls
If you’re going to conduct a reference call, the questions below will ensure you gather the required information:
- What were your denial rates and days in A/R before the engagement, and where are they now?
- How did the onboarding process go, and how long did it take to reach full performance?
- How responsive is the account management team when problems arise?
- Would you renew the contract? Why or why not?
A final tip is to always ask for anonymized before/after KPI data. A vendor that's genuinely performing well will have this readily available. One that deflects with "every client situation is different" may not have the results to share.
Step 10 — The 2026 Vendor Interview: 25 Questions to Ask
So far, we’ve covered in detail the main areas involved in assessing which vendor might be the best medical billing company for your organization. You should absolutely go through these at length before signing a contract. However, if you want a quick-reference question bank to use in a demo or evaluation call, the 25 points below will ensure you cover all the important points.
Compliance and Security Questions
- Do you have a signed HIPAA BAA template ready to share, and who are your HIPAA compliance officers?
- What access controls are in place to limit which of your staff can view our patient data?
- Can you show us a sample audit log?
- What is your documented breach notification process and timeline?
- Do you use subcontractors for any billing or coding functions? Are they HIPAA-covered?
Coding and Operations Questions
- How many of your coders hold active AAPC or AHIMA certifications?
- Can you provide references from practices with our specialty and payer mix?
- What is your internal coding QA process, and how frequently are charts audited?
- What is your current measured coding accuracy rate across clients?
- Who owns the denial management process end-to-end, and what is your current denial overturn rate?
Technology and Data Questions
- Which EHR and practice management systems do you integrate with directly?
- Which clearinghouses do you use, and do you have direct connections with our top payers?
- What claim scrubbing rules are applied before submission, and can you show us in a live demo?
- How is patient data transferred if we end the engagement?
- What is your plan for system downtime, and how is continuity maintained?
Reporting and Account Management Questions
- What KPIs do you report on, and how are they defined?
- How frequently are reports delivered, and do we have real-time dashboard access?
- Who is our dedicated account manager, and what is their caseload?
- What is the escalation path if we have a serious concern or performance issue?
- Can you share a sample reporting dashboard or anonymized performance data?
Pricing and Contract Questions
- What is included in your quoted rate, and what services carry additional fees?
- Is there a setup or implementation fee?
- What are the contract term length and termination notice requirements?
- Is there an early termination penalty?
- What does the off-boarding and data transition process look like at contract end?
Next, let’s take a look at red flags that may pop up in your search for the best medical billing outsourcing company.
Step 11 — Red Flags: When to Walk Away Fast
Not every vendor is worth a second conversation. These are the most common warning signs that signal a poor fit or potentially problematic partnership.
- Vague answers on compliance - "We take HIPAA very seriously" is not a compliance program. If you can't get specifics on access controls, audit trails, or their BAA, stop.
- No SLA or undefined KPI commitments - A vendor unwilling to commit to measurable performance targets has no accountability structure.
- "We work with every specialty" - Deep specialization matters. A vendor claiming equal expertise across all care settings almost certainly has shallow expertise in most of them.
- No reporting samples - Any established vendor should have anonymized dashboard examples or benchmark data. Refusing to share these is a red flag.
- Unclear denial ownership - If it's not clear who owns the denial appeal process and when they escalate, denials will fall through the cracks.
- Pressure to sign quickly - Artificial urgency in a contract of this importance is a negotiating tactic, not a business necessity.
- No client references in your specialty - Always require this. A vendor that can't provide them likely doesn't have a relevant track record.
Remember, the process for how to choose a medical billing service isn’t just about confirming that they can meet all your basic requirements. It’s also about ensuring that the vendor has integrity and ideally offers best-in-class services for your specialty and facility type.
Step 12 — Scorecard: How to Compare Billing Companies Side-by-Side
Most providers evaluate vendors through gut feel and sales impressions. A weighted scorecard removes that subjectivity and creates a defensible comparison to ensure you pinpoint the best medical billing company. Here's how to use the scorecard.
Score each vendor from 1–5 on every criterion, multiply by the weight, then total the scores. The highest score wins. But be sure to review any category where a vendor scores 1–2 carefully regardless of their total.
Score 1 = does not meet expectations. Score 5 = exceeds expectations with documented proof. Weight × score gives a points total per category; sum all categories for a final vendor score out of 500.
Best Medical Billing Vendor Scorecard
This medical billing company checklist and scorecard is what separates a thorough evaluation from a vendor relationship that becomes a problem six months in.
Step 13 — Implementation and Onboarding: What a Good Transition Looks Like
Onboarding hiccups happen with almost every medical billing company change. The question isn't whether there will be friction - it's whether your vendor has a structured plan to manage it.
A well-run onboarding typically follows this sequence:

Before go-live, it’s recommended to obtain a documented SOP for your account, a clear escalation path with named contacts, a reporting baseline drawn from your pre-transition data, and a written go-live checklist signed off by both parties.
If your vendor can't produce a structured onboarding plan before you sign, that's a signal about how they'll operate once you're a client.
FAQs
What's the best way to choose the right medical billing company for a practice?
Start by documenting your specialty, claim volume, payer mix, and specific pain points before talking to any vendor. Use a structured evaluation process that covers compliance verification, specialty reference checks, a live tech demo, and a weighted scorecard. Require documented KPI proof, not verbal benchmarks.
How do I know if a medical billing outsourcing partner is HIPAA compliant?
Ask for a signed BAA, written security policies, proof of data encryption (in transit and at rest), a sample audit log, and a documented breach notification process. Third-party certifications like SOC 2 or HITRUST provide additional assurance. Any vendor that can't produce these documents is a compliance risk.
How quickly should I expect revenue improvements after switching vendors?
Results depend on your starting baseline and the scope of the engagement. Most practices see measurable improvement in clean claim rates and denial rates within 60–90 days of go-live, once the vendor has stabilized workflows and completed initial payer credentialing. Establish a KPI baseline before day one so you can track progress objectively.
Should I outsource medical coding too?
If your current in-house coding has accuracy rates below 95%, high denial rates attributable to coding errors, or you're in a high-complexity specialty like behavioral health, radiology, or orthopedics—yes. Outsourcing coding to a vendor with AAPC or AHIMA certified coders in your specialty can meaningfully reduce denials and improve compliance. If your coding is performing well, billing-only outsourcing may be sufficient.
Final Checklist
Here’s a final checklist to ensure you’ve covered all the essentials for choosing the best medical billing company.
- Define your needs - Specialty, volume, payer mix, pain points, staff gaps, current tech stack.
- Determine scope - Billing-only, billing plus denials, or full RCM outsourcing.
- Shortlist vendors - Use industry references, analyst rankings, and peer recommendations to build a list of 3–5 candidates.
- Conduct vendor interviews - Use the 25-question list above. Request BAA, security documentation, and reporting samples.
- Score and compare - Apply the weighted scorecard to each vendor. Eliminate any with critical gaps in compliance or specialty fit.
- Check references - Call at least two current clients per finalist. Ask for before/after KPI data.
- Review the contract - Use the 10 contract questions to negotiate key terms before signing.
- Confirm the onboarding plan - Require a written plan with milestones before go-live.
- Establish a KPI baseline - Document current performance metrics before the transition begins.
- Set 30/60/90-day review checkpoints - Hold formal performance reviews against the agreed baseline.
Conclusion: How to Choose the Best Medical Billing Company
Finding the right medical billing company in 2026 is not a decision to make on price alone or on the strength of a sales pitch. The strongest partners combine proven specialty experience, airtight compliance practices, transparent KPI reporting, and a structured onboarding process. The scorecard and question bank in this guide to choosing the best medical billing company give you the tools to evaluate any vendor on your terms—not on their own.
Start by defining your needs clearly, verifying compliance and specialty fit (with documented proof), and comparing a shortlist of vendors side by side. Then schedule demos with your top three candidates, using our question list to ensure you cover everything, finishing with the scorecard to objectively see how they measure up.
For a no-pressure conversation about how our outsourced medical billing services can help improve your organization’s revenue cycle, contact Pharmbills today. Our expert HIPAA-compliant billing team is ready to walk you through how we approach billing, compliance, and performance reporting—with proof, not promises.


![The 4 Top Pain Points for U.S. Nursing Home Providers [2026]](https://cdn.prod.website-files.com/63d9425d235def15b898f020/65df706f82c44c9b3a089725_866.avif)
%20copy.avif)



