A revenue cycle management (RCM) audit was once treated as a reactive exercise. Something providers did when a payer pushed back, when compliance concerns surfaced, or when cash flow problems forced a closer look at billing operations. But in 2026, that approach is obsolete.
Today, leading healthcare organizations use RCM audits as strategic tools to uncover revenue leakage and defend against increasingly aggressive payer algorithms. They also help providers identify billing inefficiencies, documentation gaps, denial patterns, underpayments, and operational risks.
In this guide, we’ll explain what RCM audit means and how to perform one, which areas of the revenue cycle to review and which KPIs and documents to analyze. We also provide a sample revenue cycle audit checklist and explain how audits support compliance, denial prevention, and overall financial performance. Finally, the guide covers how technology and outsourced revenue cycle management services can make the entire RCM audit process more efficient.
RCM Audit Meaning: Quick Answer for Healthcare Providers
An RCM audit is a structured review of a healthcare organization's revenue cycle. It analyzes the data, documentation, claims, payments, denials, and collections that move from patient registration through final reconciliation. The purpose is to identify where revenue is being lost, delayed, incorrectly billed, underpaid, denied, or exposed to compliance risk.
The goal and meaning of an RCM audit depend on its scope. Some audits review the entire revenue cycle, while others focus on a single area, such as eligibility verification, prior authorization, coding, charge capture, claim submission, payment posting, denial management, or patient collections.
Additional Insights
For a foundational explanation of RCM, see our article covering What is Revenue Cycle Management (RCM) and Why Is It Important for Healthcare?
Why RCM Audits Matter More in 2026
Several converging pressures have made revenue cycle audits more important in 2026 than they were in recent years.
Payer Requirements Are Becoming More Complex
Payer rules continue to grow more elaborate, and prior authorization processes are under both regulatory and technology-driven change. As a result, denial management remains a major operational burden for most healthcare organizations.
In particular, CMS has been moving toward more structured prior authorization processes, payer reporting, and API-based data exchange, but actual implementation across payers and service lines remains uneven.
Documentation Quality Affects Reimbursement and Compliance
Clinical documentation now sits at the center of both reimbursement decisions and compliance posture. Coding accuracy, medical necessity, payer-specific requirements, and audit defensibility all depend on what the clinical record actually supports. Audits that examine documentation quality usually surface issues that affect both revenue and risk at the same time.
Revenue Leakage and Underpayments Are Widespread
Most providers lack a clear picture of where revenue is being lost or underpaid. Margins are tighter, and leakage patterns that were tolerable in earlier years now matter materially. Audits give leadership the visibility into AR aging, denial patterns, underpayments, and write-offs that day-to-day operations rarely deliver.
Staffing Shortages and Administrative Costs Continue to Rise
Industry surveys continue to identify acute staffing gaps in RCM departments at healthcare provider organizations. When billing teams are stretched, small workflow problems compound into significant revenue loss that internal teams may not have the capacity to detect.
Automation and AI Help — With Caveats
Automation and AI can support the RCM audit process (and the workflows it examines), but only when underlying data quality and process controls are sound. Automated tools applied to messy data produce confident-looking outputs that hide rather than reveal real issues.
The key takeaway is that in 2026, an RCM audit should not only look backward at past errors. It should also help providers build more resilient, measurable, and scalable revenue cycle workflows.
Additional Reading
For a broader view of where revenue cycle operations are heading this year, see The Future of RCM: Revenue Cycle Management Trends To Watch In 2026.
Internal vs. External RCM Audits: What Is the Difference?
Audits in healthcare revenue cycle management broadly fall into four categories: Internal, External, Compliance, and Focused. The table below describes each in more detail.
Internal and focused audits are tools that providers control. External payer and compliance audits are events providers respond to. The quality of that response depends almost entirely on whether internal audits have already identified and resolved the issues an external auditor would otherwise find.
Deeper Comparison
For more on how audit-related billing services fit alongside broader revenue cycle work, see Medical Billing Services vs. Revenue Cycle Management: What's the Difference in 2026.
How to Perform a Revenue Cycle Management Audit
A revenue cycle audit usually moves through three phases: pre-audit planning, audit execution and analysis, and post-audit action planning and monitoring. Each phase has its own focus, deliverables, and challenges.

1. Pre-Audit Planning: Define Scope, Goals, and Risk Areas
The revenue cycle management audit should begin with a clear goal. Without one, the audit team collects data nobody asked for and produces findings that nobody can act on.
Common starting goals include:
- Reduce claim denials in a specific service line or payer mix
- Review coding and documentation accuracy
- Identify underpayments hidden in contractual adjustments
- Evaluate prior authorization workflow
- Improve clean claim rate performance
- Assess accounts receivable aging
- Prepare for an upcoming payer or regulatory audit
- Evaluate whether outsourced RCM support is needed
Once the goal is clear, the audit charter should define the scope, sample size, period under review, departments involved, systems and data sources, KPIs, documentation requirements, responsibilities, timeline, and reporting format.
Practical example - A specialty clinic with rising denials does not need to audit its entire revenue cycle to find the cause. A focused audit of eligibility verification, prior authorization, coding accuracy, and payer-specific claim edits will usually surface the problem faster and at lower internal cost than an end-to-end review.
2. Audit Execution: Collect Data and Review Revenue Cycle Workflows
With scope and goals fixed, the RCM audit team gathers the data needed to evaluate workflow performance against payer requirements, internal policies, documentation standards, coding rules, contract terms, and operational KPIs.
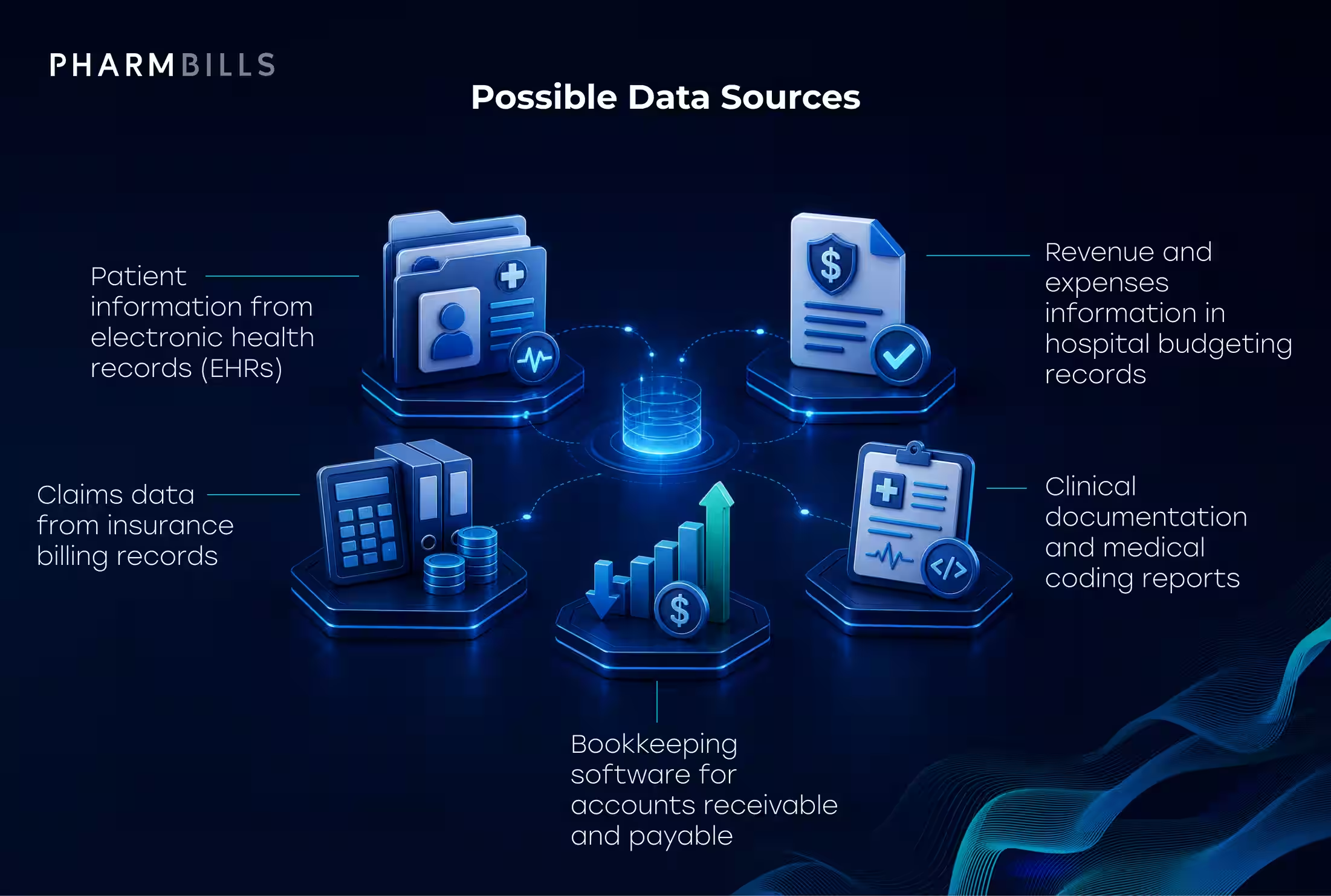
Typical data sources include:
- Patient registration records
- Eligibility verification data
- Prior authorization records
- Clinical documentation
- Coding records
- Charge capture reports
- Claims data
- Clearinghouse reports
- Payer remittances and ERA/EOB data
- Payment posting records
- Denial and appeal logs
- Accounts receivable aging reports
- Patient billing and collections data
- Contract terms and fee schedules (where relevant)
An important note on data quality: If information is fragmented across the EHR, billing software, spreadsheets, clearinghouses, and payer portals, the audit team should document those limitations explicitly rather than presenting reconciled-looking numbers that paper over the gaps. An audit that overstates data quality produces conclusions that fall apart on close review.
3. Post-Audit Review: Turn Findings Into an Action Plan
The audit report should not simply list problems. A good healthcare RCM audit report also includes:
- Key findings
- Root causes
- Financial impact
- Compliance risk level
- Operational impact
- Responsible teams
- Recommended corrective actions
- Timelines
- KPIs for follow-up
- An ongoing monitoring schedule.
The distinction that matters most is between identifying a problem and fixing the workflow that caused it.
For example, if the audit finds a high denial rate for missing prior authorizations, the action plan should not simply tell staff to "be more careful." It should review eligibility checks, payer-specific authorization rules, scheduling workflows, documentation handoffs, staff training, and pre-submission claim validation — and assign owners and deadlines for each.
More Information
Our article on Strategies for Healthcare Revenue Cycle Optimization in 2026 includes practical strategies to translate audit findings into measurable revenue improvement.
Revenue Cycle Audit Checklist: What Should Providers Review?
A practical RCM audit checklist follows the revenue cycle from front to back, so that issues caught upstream don't compound into denials and write-offs downstream. The checklist below maps each major area to what the audit should examine, what providers commonly find, and what data points or KPIs are usually involved.
This revenue cycle audit checklist is a starting framework, not a finished audit plan. The depth of review for each area should reflect the audit goal, the provider's risk profile, and any specific issues already known to leadership.
Key Components of an RCM Audit
When looking at how to perform an RCM audit, it can be helpful to consider each component of the revenue cycle.

What RCM stands for in audit includes all aspects of revenue cycle management, such as:
- Intake and prior authorizations
- Medical coding and charge capture
- Claims submission and tracking reimbursement
- Denial rates
- Payment collections
Below is an overview of the key components of an RCM audit, with examples of what data might be collected and analyzed for each.
Patient Registration and Data Accuracy
Intake and registration are the first steps of the revenue cycle, and any errors here can compound into denials, billing delays, and patient billing confusion that surface much later. By the end of registration, both the provider and the patient should have a clear picture of the financial arrangement for the planned care.
The revenue cycle audit should review:
- Demographic accuracy
- Insurance information
- Subscriber details
- Coverage verification
- Coordination of benefits
- Patient financial responsibility
- Upfront communication about expected costs
The audit RCM focus here is whether registration errors are creating denials, billing delays, or patient billing confusion that surfaces later in the revenue cycle. Front-end errors are disproportionately responsible for downstream denials, which means small improvements in registration discipline often produce outsized financial returns.
Eligibility Verification and Prior Authorization
Eligibility and prior authorization audit deserve their own attention because failures in either drive a substantial share of lost revenue.
The RCM audit should review whether:
- Authorization requirements are checked before service
- Payer-specific rules are documented
- Authorization numbers are captured accurately
- Service dates and approved units match the claim
- Documentation supports medical necessity
It’s also important to review how denied authorizations are tracked and appealed and whether authorization status is visible to scheduling, billing, and clinical teams.
Eligibility verification and prior authorization are two of the highest-leverage areas of any audit. Specialist prior authorization services can supplement internal teams when authorization volume exceeds in-house capacity or when payer-specific requirements have outpaced internal documentation.
Charge Capture and Reconciliation
Charge capture is the process of documenting services delivered so an accurate claim can be submitted. Reconciliation is matching the reimbursement received against the services billed. Errors in either create revenue leakage that often goes undetected because nobody is comparing services rendered against claims submitted.
Sources of data involved in charge capture and reconciliation include clinical documentation, medical coding reports, and billing software. In particular, the medical billing audit should review:
- Missed charges
- Duplicate charges
- Delayed charges
- Incorrect service units
- Mismatch between clinical documentation and billed charges
- Incomplete reconciliation between services rendered and claims submitted
A useful charge capture audit triangulates clinical activity, coding, billing, and payment data, not just billing data on its own.
Coding Accuracy and Documentation Support
Coding accuracy depends on documentation quality. An audit that reviews coding without examining the documentation behind it will miss most of the real issues. Coding is also a vital component of legal record-keeping in medical billing, as codes should accurately reflect the level and complexity of care delivered and billed for.
The two most common coding problems uncovered with an RCM in audit are:
- Undercoding - Codes that produce reimbursement below what the care delivered warrants.
- Overcoding - Codes that produce reimbursement above what the documentation supports.
This stage of the RCM audit requires looking at the interplay between medical coding vs medical billing. To get the full picture, the audit should review unsupported codes, modifier errors, medical necessity documentation, payer-specific documentation requirements, specialty-specific risk areas, and audit trail quality.
Claims Submission and Clean Claim Performance
Once care is delivered and coded, the next step is submitting the claim for reimbursement. Many providers use clearinghouses or medical billing specialists to "scrub" claims before submission, identifying and correcting errors before they reach the payer.
A thorough RCM audit should look at:
- Clean claim rate
- Claim rejection rate
- Missing information patterns
- Payer-specific edits
- Clearinghouse rejections
- Timely filing risk
- First-pass resolution rate
- Claim status follow-up
A high clean claim rate is a useful signal but not a complete one. A claim can pass payer edits and still be paid below contract or denied on medical necessity grounds. The audit should also look at payment accuracy, denial patterns, underpayments, and appeal outcomes, not just whether claims got through the front door.
Payment Posting and Reconciliation
Payment posting describes the time when the healthcare provider records payments received into their billing system. Payments are said to be reconciled once details of each payment (amount and payer) are allocated to individual services.
Posting errors distort financial reporting and frequently hide underpayments, because the totals can look correct in aggregate even when individual transactions are misapplied.
When conducting an audit, be sure to look at:
- ERA/EOB matching
- Contractual adjustment accuracy
- Unapplied payments
- Payment lag
- Underpayments
- Overpayments
- Secondary billing
- Patient balance transfer accuracy
- Reconciliation between the billing system and accounting records
Insights gleaned from analyzing this data are one of the main benefits of RCM audit, as it allows providers to gain a true and accurate picture of their costs vs. revenue.
Denial Management and Appeals
Some claim denials are an unavoidable cost of doing business in healthcare. But rates, follow-up speed, and appeal success vary enormously between providers, and that variance is where audits can surface compounding revenue loss.
An RCM audit usually includes analysis of:
- Denial rate by payer and reason code
- Preventable vs. unavoidable denials
- Appeal submission rate
- Appeal success rate
- Time to appeal
- Write-off patterns
- Repeat denial categories
- Denial ownership and accountability
- Root causes by workflow stage
The most common failure mode identified in this area of RCM in audit is treating denials as a counting exercise. A denial management audit should not only count denials — it should also identify why denials happen and which workflow changes would prevent recurrence. This usually means tracing denials back to eligibility, prior authorization, coding, documentation, or charge capture failures upstream.
One thing to note is that a provider may not have a high overall denial rate, but slow follow-up and a low appeal success rate can end up costing as much revenue as a higher rate would. This is exactly the type of thing a thorough audit of denial management and appeals picks up, and why audits are such a pivotal component of healthcare revenue cycle optimization.
Accounts Receivable and Collections
AR and collections audits show whether the organization is collecting revenue efficiently and consistently, or whether revenue is sitting in aging buckets that erode each month. This includes both insurance receivables and the patient-side collections, which have grown significantly with the spread of high-deductible plans.
Every revenue cycle audit checklist should include prompts to review:
- AR aging by payer
- AR aging by service line
- Days in AR
- Old unpaid claims
- Stalled claims
- Patient balances
- Collection workflows
- Bad debt trends
- Follow-up cadence
- Write-offs
Specialist accounts receivable services are commonly engaged when internal teams cannot keep pace with aging AR, particularly when high-deductible plan growth has made patient balance follow-up a larger share of total collections work.
Key RCM Metrics to Check During an Audit
A solid RCM audit is supported by measurable data, not just by manual review of claims and workflows. To properly understand what is RCM in audit, teams should select a focused set of KPIs to understand where revenue is delayed, denied, underpaid, written off, or stuck in accounts receivable.
Examples of metrics commonly reviewed during an RCM audit include:
- Clean claim rate
- Initial denial rate
- First-pass resolution rate
- Days in AR
- AR over 90 days
- Net collection rate
- Claim rejection rate
- Appeal success rate
- Payment lag
- Prior authorization-related denials
- Eligibility-related denials
- Coding-related denials
These metrics behave differently in hospital and physician practice settings. Days in AR, for example, runs naturally higher for hospital systems with complex inpatient billing than for ambulatory practices with simpler claim mixes. The audit should benchmark against peers in the same setting and specialty rather than against a single industry-wide average.
Further Reading
For deeper reading on which KPIs to prioritize and how to interpret them, Revenue Cycle Management Metrics: Which KPIs Matter Most in 2026 covers benchmarking, calculation, and trend analysis in more detail.
Common Revenue Leakage Sources an RCM Audit Can Reveal
Industry analyses consistently put combined revenue leakage at up to 7% of net patient revenue for typical hospital operations — a margin most providers cannot absorb. Revenue leakage rarely comes from a single major billing failure. It usually comes from small repeated errors at multiple stages of the revenue cycle, compounding into significant lost or delayed revenue over time.
A good RCM audit traces leakage back to the workflow stage where it originates. The most common sources fall into a few categories.
Front-end leakage. Inaccurate patient information, missed eligibility checks, and missing or expired prior authorizations are responsible for a disproportionate share of downstream denials. Errors here are inexpensive to fix at the point of registration, but expensive to fix after a claim has been denied or recouped.
Mid-cycle leakage. Incomplete documentation, undercoding, missed charges, and payer-specific claim edits not being applied during scrubbing all create gaps between services rendered and revenue collected. Coding inaccuracies that may seem small in percentage terms produce large dollar losses at scale.
Submission and timing leakage. Delayed claim submission, claim submission errors, and timely filing failures convert collectible revenue into write-offs. Even strong upstream performance can be undermined by a submission process that lets claims age past payer deadlines.
Denial and appeal leakage. Preventable denials and weak denial follow-up are among the most expensive failures in the revenue cycle. A significant share of denied claims are never appealed and eventually written off. This is lost revenue that no front-end improvement can recover.
Payment posting and reconciliation leakage. Underpayments masked as adjustments, unapplied payments, and old AR not worked consistently all hide revenue that the provider has actually earned. Posting and reconciliation audits often surface money the organization did not realize was missing.
Patient-side leakage. When patient balances are not communicated clearly, or when point-of-service collection opportunities are missed, the cost of collection rises sharply and bad debt grows. With the continued growth of high-deductible plans, patient balance management has become a larger share of total collections work and a larger source of leakage.
Practical Insight
A common audit experience is that a provider may believe their main issue is "payer denials," but an audit often reveals that the real root cause starts earlier. The source of revenue leakage could be incomplete insurance verification, missing prior authorization details, or documentation that does not support the billed service. This is why treating denials only at the payer level often leaves the underlying leakage in place.
How to Prepare for Payer Audits and Documentation Reviews
Healthcare providers should not wait for a payer audit request to organize documentation, billing records, and internal workflows. Audit readiness is always best built in advance, through documentation discipline, ongoing monitoring, and regular internal review.
Payer audits typically focus on whether services were medically necessary, properly documented, correctly coded, and billed according to payer rules. Good preparation falls into these three overlapping areas.
- Documentation discipline. Maintain complete clinical documentation, keep authorization records easily accessible, match billed services to medical necessity documentation, and document coding decisions — especially for high-value or specialty-specific codes. The goal is to ensure that any claim selected by an auditor can be defended with the underlying record.
- Tracking and monitoring. Track payer communications, monitor high-risk services, review outlier billing patterns proactively, and maintain audit trails in billing and EHR systems. Many payer audits are triggered by statistical outlier patterns. Reviewing your own data the way an auditor would helps surface issues before the auditor does.
- Training and internal review. Train staff on payer-specific requirements, particularly when payers update their policies or when new service lines come online. Conduct regular internal reviews so that a payer audit is not the first time anyone has examined the records in question.
Remember, audit-ready documentation is not the same as defensive documentation. The aim is not to produce more paper, but to ensure the paper that exists actually supports what was billed.
Deep Dive
For practical detail on prior authorization workflows, see The Ultimate Step-By-Step Guide to Prior Authorization.
The Impact of RCM Audits on Healthcare Providers
A useful RCM audit produces positive outcomes that show up in financial reporting, compliance posture, and day-to-day workflows. Here are the areas where the impact is most visible.
Better Financial Visibility
Audits help providers understand where money is delayed, lost, written off, underpaid, or stuck in AR, and at what magnitude. Without that visibility, leadership decisions about staffing, technology investment, and contract negotiation are made on incomplete data. With it, those decisions can be tied to specific revenue gaps and expected returns.
Fewer Preventable Denials
RCM audits surface denial patterns tied to eligibility verification, prior authorization, coding, documentation, timely filing, medical necessity, and payer-specific claim requirements. Once those patterns are visible, prevention becomes a workflow design problem rather than an appeals volume problem. Providers that focus exclusively on appealing denials after the fact rarely reduce overall denial rates, while providers that audit upstream causes typically make good progress in this area.
Stronger Compliance and Documentation Discipline
OIG compliance guidance — including the General Compliance Program Guidance and segment-specific guidance — provides a useful ongoing reference for identifying healthcare risk areas. Audits that align with these reference points help providers strengthen their healthcare billing compliance posture without overengineering controls. (Note: This is not legal advice. Specific compliance questions should be reviewed with qualified legal counsel.)
More Efficient Billing Operations
Audits act as a baseline for billing workflow optimization, surfacing where teams lose time through rework, manual follow-up, duplicate tasks, unclear ownership, or fragmented systems. A workflow audit that quantifies the per-claim cost of rework (which can be substantially higher in hospital settings than in physician practices) often makes the case for process changes that earlier qualitative observations could not.
Better Patient Financial Experience
Audit findings can directly improve patient communication, cost estimates, billing clarity, payment options, and the rate of surprise billing issues caused by internal errors.
Here are two practical illustrations:
- Streamlining intake and prior authorization. Cleaner intake reduces staffing costs, minimizes claim denials, and produces a faster, easier patient experience with clearer information about treatment costs.
- Adding administrative support for clinical documentation and coding. With better support, error rates in coding usually fall and clinicians spend more time on billable work (capacity that can go toward serving more patients rather than reworking claims).
In both cases, the financial gain for the provider and the experience gain for the patient move in the same positive direction. The RCM audit findings that produce changes like these tend to outperform changes that improve revenue at the risk of creating a worse patient experience.
Technology's Role in Modern RCM Audits
Technology has changed what RCM audits can examine, how quickly they can produce findings, and how much of the underlying work can be automated. But it has not changed the importance of human judgment.
EHR, Practice Management, and Billing Software Data
Modern revenue cycle audits rely on data from EHRs, billing platforms, clearinghouses, payer portals, accounting systems, and reporting dashboards. Better systems make audits faster and more comprehensive — but only if the underlying data is accurate, standardized, and consistently maintained.

When data is fragmented across disconnected systems, the audit team often spends more time reconciling sources than analyzing findings. In these cases, the audit itself becomes a useful diagnostic of data infrastructure. For example, if the audit cannot produce a clean view of denials by payer or AR by service line with a reasonable effort, that is itself a finding worth surfacing to leadership.
Automation in Claims, Denials, and Audit Monitoring
Automation now reliably supports a number of revenue cycle activities that audits draw on, including:
- Eligibility verification
- Claim scrubbing
- Denial categorization
- Payment posting
- Underpayment detection
- AR prioritization
- Reporting dashboards
- Recurring audit alerts
Used well, automation lets audit teams identify patterns faster and respond to issues continuously, rather than only during periodic reviews. Some larger health systems now use automated pre-bill review to flag anomalous claims for human attention before they ever reach the clearinghouse. This continuous-audit posture was impractical even a few years ago.
It’s important to remember that automation does not replace human oversight. It only surfaces the patterns that humans then need to interpret, prioritize, and act on.
AI in RCM Audits: Useful, but Not a Magic Fix
The question is no longer whether AI has a role in RCM — it absolutely does. In 2026, the questions are where can AI meaningfully improve audit quality and where does it introduces risk that requires additional oversight.
Where AI can help with RCM audits:
- Pattern detection
- Anomaly detection
- Documentation review support
- Denial prediction
- Workflow prioritization
Used as a tool that surfaces candidates for human review, AI can substantially improve the speed and reach of an audit team.
Where AI introduces risk:
- Coding from incomplete documentation. AI tools that recommend high-level codes from thin or contradictory documentation can introduce systematic upcoding exposure.
- Automated appeals against algorithmic denials. Bots responding to bots tend to produce a machine-vs-machine loop that resolves nothing.
- Scanning records for legacy diagnosis codes. Surfacing historical conditions without verifying active treatment during the encounter creates exactly the kind of risk-adjustment exposure that draws external scrutiny.
Providers should avoid relying on AI-generated outputs without human validation, especially for coding, documentation, compliance, and payer appeals. The most effective current model places AI in support of human judgment — not in place of it.
More Information
For more on how technology is reshaping medical billing operations in 2026, read our article on How Technology Is Transforming Medical Billing in 2026.
How Often Should You Conduct an RCM Audit?
How often you should audit RCM operations depends on provider size, specialty, payer mix, risk level, denial trends, internal resources, and recent operational changes. There is no single right cadence, but there are useful starting points.
Providers with rising denials, aging AR, frequent underpayments, payer disputes, rapid growth, new locations, new service lines, or billing team turnover should expect to audit more often.
It’s also worth noting that industry guidance has shifted in recent years toward continuous, risk-based auditing rather than a single retrospective annual review. This is especially true for organizations operating in heavily audited segments such as Medicare Advantage, post-acute care, and behavioral health.
The principle to follow is that audit frequency should match audit risk. The higher the risk, the more often the audit.
Challenges and Best Practices in RCM Audits
The hardest part of an RCM audit is rarely the analytical work. It's everything around it, such as getting clean data from fragmented systems, securing engagement from teams already stretched thin, and translating findings into workflow changes that actually get implemented.
Common RCM Audit Challenges
These obstacles show up in most RCM audits, regardless of provider size or specialty. Some are technical, but most are organizational.
- Incomplete or inconsistent data. When the same metric produces different numbers from different systems, audit findings become contestable rather than actionable.
- Fragmented systems. Data spread across EHRs, billing platforms, spreadsheets, clearinghouses, and payer portals slows the audit and weakens its conclusions.
- Unclear ownership. Without explicit accountability between clinical, billing, and administrative teams, problems surface in audits but never get fixed.
- Resistance from staff. Audits add work to teams that are usually already stretched. Without clear communication of purpose and expected outcomes, participation suffers.
- Lack of KPI visibility. When leadership cannot see operational metrics in near real-time, audits become the only visibility. However, they happen too infrequently to drive timely change.
- Poor documentation. Coding accuracy, medical necessity, and payer-specific compliance all rest on documentation. Audits that surface documentation gaps are often diagnosing a deeper training or workflow problem.
- Payer-specific complexity. Each major payer has its own edits, rules, and audit triggers. Audits that ignore payer-specific patterns miss most of the actionable findings.
- Limited internal audit capacity. Smaller teams cannot maintain the cadence of focused audits that the current environment demands.
- Findings without follow-through. An audit that identifies problems but does not lead to workflow changes is reporting work, not improvement work.
- Overreliance on manual spreadsheets. Audits assembled in spreadsheets are slow, error-prone, and difficult to repeat. This undermines the longitudinal comparison that makes audits useful.
- Narrow focus on denials. Denial-only audits miss underpayments, AR aging, and charge capture failures that often represent more significant revenue loss.
Engaging staff well is the single most important non-technical factor in audit success. The work involves participation from receptionists, data-entry staff, clinical teams across multiple specialties, and accounting and finance professionals. Treating the audit as a team effort, communicating its purpose clearly, and acknowledging the additional load all materially affect outcomes.
See The Crucial Role of Revenue Cycle Management Training in Achieving Financial Success in Healthcare for more on building the team capability that supports audit-ready operations.
RCM Audit Best Practices
The best practices below help to overcome most challenges healthcare organizations will face regarding RCM audit. They group naturally into the three phases of an audit, with each phase having its own discipline.
Before the audit:
- Define the audit goal before collecting data.
- Start with high-risk and high-value areas.
- Use consistent KPI definitions across systems and teams.
- Use a clear revenue cycle audit checklist.
During the audit:
- Review both financial and operational data.
- Trace problems back to root causes rather than stopping at symptoms.
- Involve billing, clinical, administrative, and finance teams.
- Review payer-specific rules and contracts where relevant.
After the audit:
- Document findings in a format leadership can act on.
- Assign owners and deadlines for corrective actions.
- Re-audit problem areas after changes are implemented.
- Consider outsourced support if internal teams lack the time, tools, or specialized expertise to act on the findings.
A medical billing audit that ends in a slide deck is not the same as an audit that ends in workflow change. The best practices above exist to ensure the second outcome, not the first.

When Should Providers Consider RCM Audit Support?
Internal staffing capacity is usually a finite resource. Providers may benefit from outside RCM audit services when one or more of the following pressures are present:
- Internal teams are already overloaded with day-to-day operations
- Denial rates are increasing without clear root cause attribution
- AR is aging beyond targeted thresholds
- Payer requirements are changing faster than internal documentation can keep up
- Staff turnover has affected billing consistency
- The organization lacks reliable, consistent RCM reporting
- Leadership needs an objective view of revenue cycle performance
- Post-audit improvements require additional billing, AR, or prior authorization capacity that internal hiring cannot deliver in time.
Outside support is most useful when it is not framed narrowly as "audit help." For example, a capable outsourcing partner may contribute across several of the operational areas an audit examines, including RCM operations, medical billing, prior authorization, accounts receivable, accounts payable, and healthcare back-office support.

Choosing the Right Partner
Selecting an RCM partner is a decision that benefits from a structured approach. For a practical framework, see 16 Important Questions to Consider Before Choosing an RCM Vendor.
RCM Audits in Healthcare: Summing Up
A healthcare RCM audit is not just a compliance exercise. It is a practical way for healthcare providers to understand where revenue is delayed, lost, denied, underpaid, or exposed to risk. Crucially, a well-performed audit also translates that understanding into specific workflow changes that improve healthcare financial performance, compliance posture, and patient experience.
The strongest audits in 2026 are continuous and risk-based, supported by the right mix of internal expertise, technology, and outside capacity. For providers operating against tight margins and increasingly aggressive payer adjudication, that discipline is no longer optional — it's the difference between a revenue cycle that holds up under scrutiny and one that doesn't.
Get Expert RCM Audit Support from Pharmbills
If your team needs additional capacity to conduct an RCM audit or to act on its findings, Pharmbills can help. We place dedicated, trained professionals directly into your existing systems and workflows, with no platform migration and no disruption.
Our team includes experts in medical billing, prior authorization, accounts receivable, payment posting, claims audits, and the broader revenue cycle operations that audits surface. Clients typically reduce operational labor costs by 40–50% compared to domestic staffing, while gaining the capacity to act on audit findings rather than letting them sit in a report.
Contact us today to discuss how we can support your RCM audit and revenue cycle operations.